Acute respiratory failure
Synonyms in a broader sense
Acute respiratory distress syndrome, acute respiratory failure, shock lung
definition
The acute lung failure (ARDS) is acute lung damage in patients with previously healthy lungs, caused by direct (in the lung located) or indirect (systemic, but not dated Heart outgoing) Causes.
ARDS is defined as follows:
- acute onset
- Fluid accumulation (=Infiltrates) in both sides of the lung (=bilateral), visible in a X-ray of the upper body ( Chest X-ray in the posterior-anterior beam path)
- Index for oxygen saturation (= oxygenation index) PaO2 / FiO2 <200mmHg
- This is also known as the Horowitz oxygenation index and indicates the quotient of the partial pressure of oxygen in the arterial (i.e., oxygen-enriched blood leaving the heart) and the proportion of oxygen in the breath when inhaled. Normally the quotient is 500 mmHg.
- Lung capillary occlusion pressure (= PCWP, wedge pressure) <18 mmHg and no evidence of increased pressure in the left heart.
- The wedge pressure reflects the pressure in the left heart and is measured using a right heart catheter. The normal range is between 5 and 16 mmHg.
A distinction is made between acute lung injury (ARDS) and ALI (acute lung injury). ALI is the milder form and only differs from acute lung failure in its definition by an oxygenation index between 200-300 mmHg.
frequency
Uniform information on acute respiratory failure absence. The dates are between 5 - 50/100000 / year.
In intensive care medicine, around 30% of patients are affected.
causes
A distinction is made between direct and indirect lung damage (acute respiratory failure)
The direct ones include:
- Inhale (=aspiration) of stomach contents or fresh / salt water ("Almost drowning ")
- Inhalation of poisonous (= toxic) gases, such as Flue gas
- Inhalation of hyperbaric oxygen
- Poisoning (= intoxication) with anesthetics
- As a result of pneumonia requiring ventilation (=pneumonia)
Indirect causes are:
- Sepsis ("blood poisoning")
- Burns
- Multiple trauma
- Fat embolism
- Replacement of blood volume with blood donated (= mass transfusion)
- Acute inflammation of the pancreas (= pancreatitis)
- shock
- Bone marrow / stem cell transplant
Acute lung failure in inflammation of the pancreas
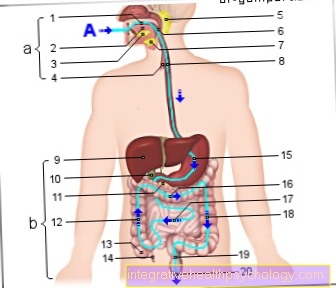
The pancreas is located in the body at the beginning of the digestive tract. It releases many enzymes that are needed to break down and digest the food ingested. The pancreas can become inflamed as a result of medication, metabolic disorders, infections or a build-up of the bile. As a result, the digestive enzymes, which are usually safely packaged, enter the pancreatic tissue and destroy it. In the case of an acute inflammation, there is severe pain in the upper abdomen, usually fever and a clearly bloated stomach are also found as symptoms.
Acute lung failure can be a complication of this condition. The permanent inflammation of the pancreas leads to what is known as consumption coagulopathy. The blood clotting system is permanently activated by constant small bleeding. After a certain period of time, the coagulation factors are used up and bleeding becomes more severe because the blood no longer coagulates. The first phase of this consumption coagulopathy is accompanied by the formation of many small blood clots that can disrupt the flow of blood in other organs. The lungs are particularly susceptible to interrupted blood flow and respond with acute lung failure.
Pathogenesis

The course of acute lung failure (ARDS) can be found in 3 stages subdivide that lead to a massive disruption of the lung tissue:
- exudative phase: The wall between the Alveoli (=Alveoli) and the Blood vessels (=Capillaries) is damaged, which increases the permeability for proteins and fluids. There are accumulations of fluid (=Edema) in the lungs.
- early proliferative phase: The lung cells (Type II pneumocytes) perish, as a result of which a deficiency in a surfactant (=Surfactant) and thus fluid in the alveoli (=Alveoli) can reach. Alveolar pulmonary edema forms. Furthermore, thin walls are formed (=Membranes) between the alveoli and the branches connecting the airways. Form in the small blood vessels small blood clots (=Microthrombi). This stage is reversible.
- late proliferative phase: The lungs are remodeled by incorporating more connective tissue (= fibrosis). This also applies to the wall between the lungs and blood. This thickens up to five times, which makes both the blood flow and the passage of oxygen into the bloodstream more difficult. This stage is irreversible and often has a fatal outcome.
Symptoms
The symptoms of acute respiratory failure are stage-specific.
In stage 1 there is a lack of oxygen in the blood (= hypoxemia) and an increased respiratory rate (= hyperventilation). This leads to shifts in the acid-base balance, the pH rises (= respiratory alkalosis).
In stage 2, the shortness of breath increases and there are spotty, streaky condensation of the lungs, which are visible in the X-ray image.
In stage 3, in addition to hypoxemia, there is an increase in the proportion of carbon dioxide (= hypercapnia), as the CO2 can no longer be exhaled enough. This is called global respiratory failure and is characterized by a falling pO2 and an increasing pCO2. The acid-base balance shifts to an acidic pH, resulting in respiratory acidosis. In the X-ray image, there are now shadows on both sides.
diagnosis
X-rays are made to monitor the progress of acute lung failure. Blood gas analysis (Taking blood from the earlobe) is required for monitoring the acid-base balance. In lung function, acute lung failure shows a decrease in the ability of the lungs to absorb oxygen (= diffusion capacity) and a decrease in lung extensibility (= compliance) at an early stage. A heart echo is performed to rule out a heart disease.
3 criteria must be met for a diagnosis to be made:
- Presence of a trigger factor
- Hypoxemia unresponsive to therapy
- X-ray evidence of changes in the lungs that cannot be traced back to cardiac pulmonary edema.
Read more on the topic: Chest x-ray (chest x-ray)
therapy
If possible, the cause of the acute lung failure should be eliminated, e.g. in circulatory shock.
Thereafter, symptomatic therapy is given. Due to the increasing shortness of breath, the patients have to be ventilated. However, since normal ventilation would damage the lungs, lung protective ventilation is used (acute lung failure). This is made up of low peak pressures and low tidal volumes. This is combined with positive pressure at the end of exhalation (= end-expiratory pressure, PEEP). As soon as the patient breathes spontaneously, assisted spontaneous breathing procedures (such as. BIPAP or APRV) used.
Alternatively, a machine can be used which eliminates CO2 outside the body (= extracorporeal) via a venovenous circulation expansion and enriches the blood with oxygen, a so-called EKMO (extracorporeal membrane oxygenator).
In severe cases, the patient is placed on the prone or in a special bed with continuous 60 ° rotation. This is a supportive measure that improves oxygen distribution.
The patient must be fed enterally.
Complications such as Infections are treated with antibiotics; in the late healing stage, corticoids improve pulmonary fibrosis.
More information is available here: The pulmonary fibrosis
The last option is a lung transplant (acute lung failure).
Artificial coma in acute respiratory failure
In the case of acute lung failure, the lungs are suddenly no longer able to supply the body with sufficient oxygen. This leads to a life-threatening situation that requires very extensive therapy in the short term. In these cases the lungs need strong mechanical support to ensure the survival of the affected person. According to current medical standards, an ECMO (extracorporeal lung membrane oxygenation) is usually used for this. The oxygen-poor blood of the affected person is passed out of the body into the machine. There it is enriched (topped up) with oxygen and then returned to the body. Since the method is highly invasive, that is, it interferes heavily with the system of the human body, affected people are usually put into an artificial coma.
In the meantime there are also more and more watch ECMOS. The affected person is conscious, can eat, drink and speak, and rehabilitation measures such as light muscle training can be started more quickly.
Read more on this topic at: Artificial coma or artificial coma for pneumonia
forecast
The lethality of acute lung failure depends on overcoming the underlying disease and the start of therapy. Pre-existing illnesses and chronic alcohol consumption worsen the prognosis.
After injuries without upper body involvement the lethality (mortality) is approx. 10%, with upper body injuries approx. 25%. If acute lung failure (ARDS) is caused by pneumonia, the mortality rate is 50%. In the case of a sepsis with multiple organ failure, even> 80%.
Further information
Further information on this topic can be found on the following pages:
- Shortness of breath
- Atelectasis
- Bronchitis
- ECMO
- Inflammation of the windpipe
- Pulmonary embolism
- lung infection
- Pneumonia after surgery
- Diseases of the lungs that are treated surgically
- Lung transplant
- Cystic fibrosis
- Pneumothorax
- pleurisy
- hiccup