What are the symptoms that can be used to recognize a diaphragmatic hernia?
introduction
Diaphragmatic hernias can be divided into congenital and acquired forms. While the acquired diaphragmatic hernia shows no drastic symptoms or can even go unnoticed, the congenital diaphragmatic hernia in infants is a serious clinical picture that becomes noticeable immediately after birth.
What symptoms can indicate a diaphragmatic hernia?
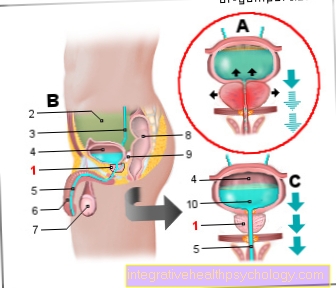
The most common symptom complex of acquired diaphragmatic hernia in adults is heartburn after eating and excessive bloating, including stomach pain. Are there any risk factors for a diaphragmatic hernia such as Obesity, pregnancy or a low-fiber diet suggests the suspicion. The diagnosis is confirmed by means of a gastroscopy. In it, parts of the stomach in the chest can be determined. A diaphragmatic hernia can also be seen on x-rays, but x-rays are rarely used for diagnosis. In the case of a complete displacement of the stomach into the chest, symptoms of the cardiovascular system can also appear, especially after eating. The displacement of the heart and lungs leads to arrhythmias, increased heart rate and shortness of breath.
Read more on this topic at: Diaphragmatic hernia
The following symptoms could indicate a diaphragmatic hernia in the baby
In babies, the diaphragmatic hernia arises in the womb due to a malformation, which is why this malformation is often detected using ultrasound during the preventive examinations during pregnancy. In the most common form of congenital hernia (Bochdalek hernia) organs have slipped through a gap in the back of the diaphragm from the abdomen into the chest and prevent the lungs from developing there. After the child is born, a specialist team of pediatric surgeons is available to care for the newborn.
Read more on this topic at: Check-ups during pregnancy
However, should a congenital diaphragmatic hernia go unnoticed, the child will be noticed immediately after birth with symptoms of lack of oxygen due to the underdeveloped lungs. The children have shortness of breath and are often cyanotic ("turned blue" due to lack of oxygen) as a sign of respiratory failure. With diaphragmatic hernias that are less large or rare, the symptoms can be very diverse. Spitting immediately after eating, screaming due to pain, or growth retardation may occur, but they do not necessarily indicate a diaphragmatic hernia. With symptoms of this kind, a pediatrician should always be consulted to rule out other malformations.
Read more on this topic at: Difficulty breathing in the baby
Are there also diaphragmatic hernias that do not cause symptoms?
The most common form of diaphragmatic hernia, acquired hiatal hernia, is symptom-free in the majority of cases. The severity of the hernia is often minor, only the narrow point at the junction of the esophagus (Esophagus) to the stomach is somewhat expanded. Frequently, a gastroscopy performed because of other complaints reveals a slight hiatal hernia as an incidental finding. Such a finding, however, has no consequences as long as there are no symptoms that can be attributed to the hernia. The extent of the therapy always depends on the patient's complaints.
You can find more about this type of hernia on our page Axial hiatal hernia
heartburn
The classic symptom of acquired diaphragmatic hernia (Hiatal hernia) is heartburn, also called reflux. Due to the expansion of the diaphragm at the passage through the esophagus, the constriction in front of the stomach entrance is missing and stomach acid runs back into the esophagus. This causes a burning and uncomfortable feeling behind the breastbone and can be accompanied by frequent belching. Long-term reflux, however, can lead to esophageal ulcers and even malignant changes. However, this can usually be prevented by taking so-called proton pump inhibitors (PPIs, e.g. pantoprazole) on a daily basis.
Read more on this topic at: heartburn
shortness of breath
Shortness of breath as a symptom of a diaphragmatic hernia in adults is rather rare and an indication that there is already a lot of abdominal organ in the chest and displacing the lungs. The shortness of breath does not occur suddenly but develops over time. It is usually associated with heartburn and a feeling of fullness and sometimes gets worse after eating. In the event of sudden and persistent shortness of breath without symptoms from the gastrointestinal tract, a doctor should be consulted urgently, as it may be a pulmonary embolism or a heart attack. In babies, however, shortness of breath after birth is typical of a congenital diaphragmatic hernia and should be examined immediately and treated surgically.
Read more on this topic at:
- Shortness of breath
- Difficulty breathing in the baby
Bleeding
If the stomach lies partly in the chest and partly in the abdominal cavity, the constriction of the stomach in the diaphragmatic gap can lead to chronic irritation of the mucous membrane in these areas. This irritation develops into ulcers over time, which can also bleed. The residues of this bleeding can be noticed in the form of coffee grounds-like, dark flakes when vomiting. Life-threatening, insatiable bleeding in the stomach is extremely rare with diaphragmatic hernias. Taking PPIs also helps here, but surgical treatment should be considered at such a stage.
Read more on this topic at: Gastrointestinal bleeding
Anemia
The oozing bleeding in ulcers of the gastric and esophageal mucosa can lead to anemia over a long period of time. The ulcers bleed again and again and this not only results in a certain loss of blood, but also an iron deficiency, which in turn causes anemia. This can be clearly determined in the blood count, because the anemia caused by iron deficiency is characterized by small red blood cells that are poor in hemoglobin.
Read more on this topic at: Anemia
Pinching of parts of the stomach
It is very rare for abdominal organs to become trapped in a diaphragmatic hernia. Over time, the organs are surrounded by a connective tissue cover in their new location and thus grow firmly. However, entrapment, be it from the stomach or parts of the intestine, in the hiatal hernia are known and represent a serious clinical picture. An entrapment is expressed by rapidly increasing and persistent abdominal pain, which can become unbearable. The blood supply to the pinched organ is cut off, oxygen no longer arrives and the tissue threatens to die. Rapid surgical care is essential.











.jpg)