Anaphylactic shock
introduction
Anaphylactic shock describes the maximum variant of an allergic reaction of the immediate type (type I). This is an overreaction of the immune system to various substances (e.g. bee / wasp sting, food, medication). The symptoms of an allergic reaction (itching, wheals, redness) and, in addition, a drop in blood pressure up to circulatory failure occur. In addition, shortness of breath, palpitations, urination and defecation up to wetting and defecation can occur. It is an acutely life-threatening reaction. Therefore, an emergency doctor should be alerted and first aid measures should be started. Some patients have an "emergency kit" with which they can start their own therapy on site.

Symptoms
Typical symptoms of anaphylactic shock occur immediate allergic reaction (Anaphylaxis) on. The anaphylactic reaction is divided into four stages, which should allow an assessment of the severity of the reaction. Although these stages can occur sequentially, a higher level can be reached right at the beginning. Typical symptoms of an allergic reaction are: itchingwhich can be localized as well as distributed over the whole body; wheals raised from the actual skin level (Urticae) - these can change their shape and merge; a Redness of the face (see Flush syndrome) and the skin in general Feeling hot. Also Restlessness and fear are common. Severe reactions can also cause palpitations, Drop in blood pressure, Urge to defecate, Nausea, salivation and difficulty breathing.
Shock in the narrower sense is spoken of when there is also a very low blood pressure Circulatory failure and life-threatening shortness of breath with swelling of the airways. This can also lead to unconsciousness.
In the extreme can it to Death from respiratory failure and / or cardiac arrest.
causes
Any substance that can cause an allergy can lead to anaphylactic shock. It is typical that only the second contact leads to such a reaction. Since the allergens are common substances, the first contact is often not consciously noticed. Common triggers are:
Medication:
Numerous drugs can trigger allergic reactions and even anaphylactic shock. Here, allergic reactions are relatively common, whereas anaphylactic shock as a maximum variant is relatively rare. Medicines that trigger allergic reactions particularly frequently are e.g. Antibiotics (especially those from the group of penicillins), pain relievers (such as aspirin, ibuprofen, paracetamol, metamizole) and X-ray contrast media.
Food:
Many foods also cause allergies. Allergies to nuts, soy and shellfish (e.g. lobsters, crabs, mussels) are particularly common. Local differences in the frequency of such allergies can be determined. Peanut allergy is more common in the US than in Europe. This is attributed to the high consumption of peanut butter.
Insecticides:
Bee and wasp stings can often trigger anaphylactic reactions. We speak of an allergic reaction if the swelling of the puncture site is more than 10 cm and additional symptoms of an allergic reaction occur.
Also read our topic: Allergic shock
Latex:
Anaphylactic reaction can be triggered, especially when inhaling dust containing latex. Frequent contact with latex leads to a higher risk of developing a latex allergy. Therefore, people who come into frequent contact with latex at work are particularly affected (especially in the medical field, as many disposable gloves are made from latex).
Pollen:
Pollen is often the cause of runny nose and tears in the eyes in the context of allergic rhinoconjunctivitis. Rarely, they can also lead to anaphylactic reactions.
Infections:
Bacterial components can also cause severe allergic reactions in the context of infections. These can also occur during antibiotic therapy, when the bacteria break down and many bacterial fragments get into the blood.
therapy
If there are signs of anaphylactic shock, one should be contacted immediately Emergency doctor be called because it is a life threatening condition acts that require immediate therapy.
The most important action taken in an anaphylactic reaction is Removal of the allergen (as far as possible).
As a first aid measure, it should first be checked whether the person is still breathing and whether the circulation is still working. If this is not the case you should contact one immediately revival to be started.
To stabilize the circulation is the so-called Shock position makes sense. To do this, the person is laid flat on the floor and their legs are raised to facilitate the return of blood from the legs to the body.
Therapy by the emergency doctor depends on the severity of the allergic reaction. Often enough for slight reactions Gift one Antihistamine, as well as the administration of a cortisone (glucocorticoid). Circulatory instability can be caused by the Giving fluids as an infusion be counteracted. In the event of shock, adrenaline can constrict the blood vessels, which increases blood pressure.
For additional asthmatic complaints, a Asthma spray (Emergency spray / short-acting betamimetic) can be used. If breathing problems arise due to the swelling of the airways in the throat, one may also be Ventilation by the emergency doctor become necessary.
Emergency kit
People who are known to have an allergy with strong reactions such as anaphylactic shock are often given a so-called "emergency kit" for self-therapy. It is an antihistamine and a cortisone preparation. These can then be taken in an emergency situation. Such a set also includes an adrenaline autoinjector, which can only be used after prior training. This is a pre-filled syringe that injects adrenaline into the thigh muscle by pressing firmly on the thigh. It is important not to touch the top of the auto-injector to prevent accidental injection into the finger!
Also read that Articles on the topic: First aid
diagnosis
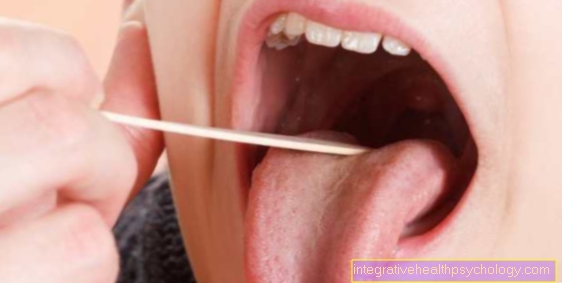
In acute anaphylactic shock, the diagnosis is usually based on the typical symptoms, often together with a typical trigger such as a bee sting or an antibiotic you have just taken. In order to prove an allergy after an allergic reaction, the further Diagnosis by a dermatologist be useful. For this purpose, possible triggers and typical symptoms are first asked in a detailed conversation and put into context. In addition, a Reaction to typical allergens evoked become. These tests all carry the risk of a severe anaphylactic reaction and should therefore only be performed by an experienced, on-call doctor. The most frequently used test is the "Prick test": To do this, standardized allergens are dropped on the forearm and then the skin is pierced with a small lancet. After approx. 20 minutes you can read off which allergens were reacted to (a wheal with reddening is considered a reaction). However, through this test just an awareness to be detected on the substance. It does not show which symptoms this substance causes.
At a "Scratch test“The skin is scratched about 1cm long and the suspected allergen is then dripped on or rubbed in. If these tests do not indicate sensitization and there is still a strong suspicion of an allergy, the allergen can also be injected into the skin of the back with a syringe. However, this test is associated with a higher risk of an anaphylactic reaction.
Furthermore, blood tests are included Determination of antibodies against possible allergens possible (total IgE and specific IgE). In some cases, direct provocation with the triggering substance can also be considered. However, this should be done very cautiously after an anaphylactic shock.
forecast
Anaphylactic shock is a life-threatening situation that requires immediate treatment. The prognosis depends on the severity of the allergic reaction and the time to start therapy. Therefore, people who have had an anaphylactic shock are given an emergency kit and trained in its use.
prophylaxis
The best way to avoid another anaphylactic reaction is this Avoidance of the triggering substance. With some allergy triggers there is the possibility of a desensitization (also called specific immunotherapy). This is especially used for wasp or bee venom allergies. It is also possible with individual pollen that cause allergic asthma or hay fever. It is mainly used when the symptoms are less than 5 years old and in younger patients. For this purpose, the specific allergy-causing substance injected into the skin in a very small dose (or put under the tongue). The dosage is increased over at least three years. The immune system is supposed to get used to the allergen. The success rate is up to 65% and is particularly favorable in young patients and allergies to only one trigger.
Some studies have shown that infants who are breastfed in the first 6 months of life have a lower rate of allergies. In children whose parents suffer from allergic reactions and who cannot breastfeed, a diet with so-called hypoallergenic milk formula can be considered.