Axial hiatal hernia
definition
A hiatal hernia refers to the displacement of parts of the stomach into the chest cavity through the opening in the diaphragm. Usually the esophagus lies in this opening and the stomach only begins below it. The axial hiatal hernia is a sliding hernia. The upper part of the stomach slides through the opening into the back of the so-called mediastinum. This refers to the area in the chest between the lungs. Older, overweight people are more often affected. In many cases, those affected have no complaints.
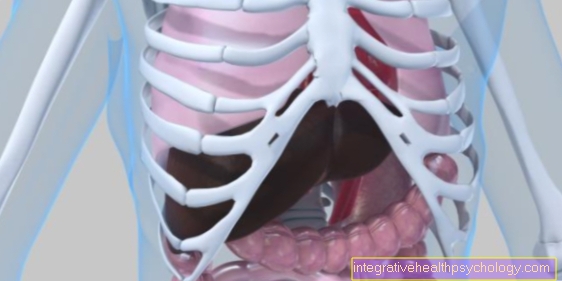
What forms are there?
There are different forms of diaphragmatic hernia. One form is the axial hiatal hernia, in which the upper part of the stomach, also known as the cardia, slides up through the opening of the diaphragm. This form is more common than other forms. There is also the paraesophageal hernia. Here, parts of the stomach clamp next to the esophagus in the opening of the diaphragm, while the transition between the esophagus and stomach is normally located in the abdominal cavity. The trapped stomach parts can lead to bleeding and passage disorders.
Axial hiatal hernia
Another name for the axial hiatal hernia is sliding hernia. Most of the esophagus is usually in the chest cavity and about two centimeters below the diaphragm is where it meets the stomach. In the case of an axial hiatal hernia, this relationship shifts. The lower two centimeters of the esophagus and the transition to the stomach slide up into the chest cavity. The displaced parts of the organ slide along the normal, anatomical axis, giving the axial hiatal hernia its name. Older and overweight people are particularly affected by this type of hiatal hernia.
Loosening the diaphragm, which is a muscle, at the site of the opening can increase the likelihood of an axial hiatal hernia. A deformed junction between the stomach and esophagus can also be a risk factor.
Most of those affected have no symptoms from the hernia and are often unaware of its existence. In some cases, heartburn, chest pain, and difficulty swallowing occur. Therapy is only necessary if there are symptoms. In this case, conservative therapy with acid blockers is tried first and surgery is only carried out in extreme cases. The axial hiatal hernia is the most common type of hiatal hernia and often goes undetected and symptom-free.
Paraesophageal hernia
The paraesophageal hernia is a rarer type of hiatal hernia. As with the axial hernia, parts of the stomach are shifted into the chest cavity, but the transition between the esophagus and stomach remains in the abdomen. Both the esophagus and the stomach are located in the opening of the diaphragm and the stomach can be pinched. This can lead to bleeding in the stomach or even anemia. In extreme cases, it comes to an upside-down stomach. This means that the entire stomach lies in the chest cavity and, in addition to stomach problems, breathing disorders can also arise. Stomach entrapment requires treatment.
causes
As with almost all clinical pictures, there is no single cause for hernias, rather it is an unfortunate combination of many factors. With age, the tissues and muscles become weaker. The diaphragm is also a muscle. As the muscles weaken, the opening of the diaphragm also loosens and allows additional contents, such as the stomach, to pass through more easily. Obesity is another important factor in the development of diaphragmatic hernias, as there is great pressure on the diaphragm, especially when lying down, and the organs, in this case the stomach, use weak points to evade. The process of pregnancy is similar. A hernia can also develop if the abdominal pressure increases significantly, for example when pressing. In addition, congenital malformations can pose a risk. The junction between the stomach and esophagus usually has a certain angle, the so-called His angle. If this angle is steeper, it will be easier for the stomach to slide through the opening. Various diaphragmatic malformations also lead to congenital hernias. Much of the paraesophageal hernia arises from such developmental disorders.
diagnosis
In many cases, the existence of an axial hiatal hernia is not known to those affected because it usually does not cause any symptoms. Sometimes gastrointestinal noises in the chest area can be heard while listening. For symptoms such as heartburn, a gastroscopy can be done, which can reveal the hernia. An X-ray examination with contrast media is also suitable for diagnosis. In gastroscopy for other reasons, the hiatal hernia can be found incidentally and therefore does not necessarily have to be treated. The patient's medical history is important, as previous hernias are very likely to relapse.
Symptoms of axial hiatal hernias
In many cases, axial hiatal hernias are completely asymptomatic, which means that the person concerned has no symptoms. Common symptoms of hiatal hernias are heartburn and a feeling of pressure in the chest. As the transition glides up, the lower esophageal closure mechanism no longer works and stomach acid can flow up, especially when lying down, causing heartburn. The feeling of pressure comes from the additional mass in the chest cavity.
With larger parts of the stomach in the chest cavity, the space occupation can also cause shortness of breath, as the stomach restricts the lungs. Swallowing disorders are also a possible symptom, which occurs due to the narrowing of the stomach in the diaphragmatic opening.
In addition to the hernia, many sufferers also have gallstones and diverticulosis, i.e. small protrusions of the intestinal wall. Although the connection has not been clarified with certainty, there is a significant accumulation of these three clinical pictures together and doctors speak of the Saint Trias. In rare cases, entrapment occurs, which disrupts the blood supply and leads to ulcers and bleeding in the stomach, which are associated with pain, nausea and anemia. These consequences are much more common in paraesophageal hernia.
You can find more about the symptoms on our website Symptoms of a diaphragmatic hernia
Reflux esophagitis
Normally, the esophagus at the junction with the stomach forms a muscular ring at the junction with the stomach, preventing stomach acid from flowing back into the esophagus. This process is supported by the diaphragm at the point of passage through the esophagus. However, if the transition between the esophagus and stomach slides over the diaphragm, this support of the locking mechanism is missing. Especially when lying down, stomach acid refluxes into the esophagus and causes heartburn. The mucous membrane of the esophagus, unlike that of the stomach, is not equipped with protective measures against the body's own acid.
The stomach acid attacks the mucous membrane and leads to inflammation and ulcers, which in extreme cases can turn into malignant tumors.
So-called reflux esophagitis requires treatment. In most cases, acid inhibitors such as pantoprazole are given first to reduce acid production in the stomach. When diagnosing chest pain, to be on the safe side, a possible heart attack should always be ruled out, as the acute symptoms can be similar. If conservative therapy does not improve, surgical therapy should be considered.
Pain
The axial hiatal hernia only rarely causes stomach pain itself. However, people may have reflux esophagitis and develop severe heartburn and chest pain. These can usually be dealt with with acid blockers. Possible circulatory disorders can also trigger pain. A circulatory disorder with subsequent death of parts of the stomach is very rare in axial hernias and is more common in paraesophageal hernias. If the chest pain is unclear, a possible heart attack should always be excluded.
Heart trouble
Both forms of hiatal hernia can lead to heart problems in extreme cases, as large parts of the stomach represent a mass in the chest cavity and thus the heart may be constricted. This leads to circulatory problems and also shortness of breath. Those affected are usually operated on directly and monitored by intensive medical care. It is more common that the pain of reflux esophagitis is initially classified as a heart condition, since the acute pain is quite similar.
Bad breath
Bad breath is a common symptom of reflux esophagitis. Those affected often have to burp and the stomach acid can smell unpleasant. If there are already ulcers in the esophagus, these damaged areas of the mucous membrane can also cause bad breath. This bad breath comes from the esophagus and therefore cannot be prevented by intensive oral hygiene. Due to its social component, bad breath can represent a severe restriction for those affected and therefore also be an indication for surgery.
treatment
Asymptomatic axial hiatal hernias, which can be an incidental finding, do not necessarily have to be treated. For mild symptoms such as heartburn, changing your sleeping position can be helpful. Elevating the torso reduces the flow of stomach acid back into the esophagus. In the case of reflux esophagitis, i.e. inflammation of the esophagus due to persistent acid reflux, the acid production can be inhibited with medication. So-called proton pump inhibitors, such as pantoprazole, inhibit the production of hydrochloric acid in the stomach and less acid can flow up the esophagus.
In the case of severe complaints, such as a restriction of the lungs and heart or a circulatory disorder in the stomach, an operation is necessary. The relocated parts of the organ are covered through the fracture site and the upper part of the stomach is sewn to the diaphragm. This can prevent relapse. In the case of very large defects in the diaphragm, a plastic mesh can also be sewn in to prevent the abdominal organs from sliding up. In acute operations, especially in the paraesophageal hernia, intensive medical care is necessary after the operation and newborns must be ventilated.
nutrition
Since the axial hiatal hernia is often accompanied by reflux esophagitis, this determines the diet. Meals should be more regular and smaller. Highly acidic foods should be avoided. Even very high-fat foods increase acid production in the stomach. Well-known triggers of heartburn include fruit juices, alcohol, coffee and all fatty foods. Those affected should not eat immediately before going to bed, as the change in position of the body also promotes reflux. The hernia itself is not a reason for a special diet.
More detailed information and nutrition tips can be found in our article on the subject Diet for heartburn
When is an operation necessary?
The need for an operation on an axial hiatal hernia depends on the severity of the symptoms. If symptoms, such as heartburn, cannot be treated conservatively, surgery may be considered. If there are complications, i.e. a constriction of the heart and lungs or a circulatory disorder in the stomach, an operation must be performed. The paraesophageal hernia is always an indication for surgery, as breathing is restricted and parts of the stomach can also die.
Course of the operation
There are different options for the operation depending on the type of hernia. The operations are always performed under general anesthesia. With the exception of the emergency operations, there is a discussion with the responsible anesthetist before the operation so that the anesthesia can be planned individually.
If only gastric acid reflux is to be prevented, narrowing the esophagus may be sufficient.
In the normal axial hiatal hernia, the stomach is first returned through the opening of the diaphragm. The surgeon pays attention to possibly undersupplied and dead parts of the stomach, as these would have to be removed to prevent blood poisoning. The opening of the diaphragm is narrowed and stabilized with a ring to prevent new hernia formation. In addition, the top of the stomach is sutured to the diaphragm, thus stabilizing the position in the upper abdomen.
In the case of larger defects of the diaphragm, such as the congenital paraesophageal hernia, a plastic mesh can be sewn in to prevent the abdominal organs from shifting. These operations require intensive medical care afterwards, while a normal ward is sufficient for follow-up treatment with a normal axial hernia.
Surgery Risks
Like all operations, hernia surgery is associated with risks. General anesthesia brings some risks with it, such as intolerance to the anesthetic drugs and ventilation difficulties. In addition to these general operational risks, every operation has its own specific risks. Hernia surgery can damage nerves and vessels in the stomach and diaphragm. If the phrenic nerve, the diaphragmatic nerve, is injured, it can cause breathing difficulties. In the vagus nerve, the nerve of the parasympathetic nerve, gastric emptying disorders can occur. However, complications are rare with these operations.
Duration of an operation
Simply narrowing the esophagus to prevent reflux esophagitis is a very brief operation. The actual hiatal hernia operation is a somewhat more complex operation that in some cases also has to be performed on the open abdomen. The exact duration of the operation cannot be determined as it varies from person to person. Afterwards, a hospital stay of around five days can be expected.
forecast
The prognosis for an axial hiatal hernia is very good. The result of the operation is checked again with an X-ray examination with contrast agent and the affected person can usually leave the hospital after a few days.
In the case of congenital diaphragmatic defects with a paraesophageal hernia, the prognosis is worse. In complicated cases, around 40% of newborns die.









.jpg)