Inflammation of the chest
General
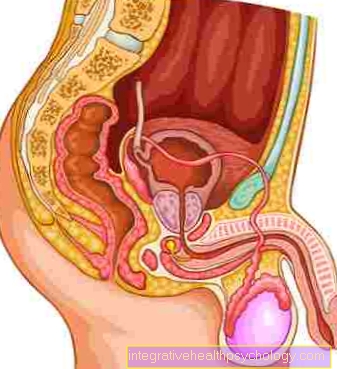
The inflammation of the breast or the mammary gland (Greek "mastos") is called mastitis or mastadenitis. For the most part, it affects breastfeeding women shortly after giving birth. This period of time is known as the puerperium. Inflammation of the breast outside the puerperium is less common. Breast inflammation in men is also a rather rare case. Mastitis requires immediate medical attention to prevent complications. This primarily involves preventing a mature abscess from developing. An abscess is an encapsulated collection of pus in tissue. There are different types of mastitis, with slightly different symptoms and causes.
Read more about this: Breast abscess
Symptoms

Inflammation of the chest does not go unnoticed. It is very often expressed in Pain in the field of nipple. Mostly the pain one-sided. It comes to fever and overheat the affected breast. The chest is red and swollen. This swelling is also palpable. The Lymph nodes The armpit may also be swollen. Ultimately, the inflammation also affects the quality of the Milk secretions noticeable. It is changed and the number of cells in it is increased.
Causes and classification
In general, bacterial pathogens cause mastitis. Classically, these pathogens include bacteria that also occur in normal skin and oral flora. These are sometimes staphylococci, streptococci and Pseudomonas.
There are different types of mastitis. There is puerperal mastitis, which occurs during the so-called puerperium, non-puerperal mastitis and periductal mastitis. They are explained in more detail below.
Inflammation of the breast during menopause
In 60% of women, mastitis occurs before the age of 30, usually before menopause. Inflammation of the mammary glands during menopause is therefore rare.
You might also be interested in: Signs of menopause
Changes in the hormonal balance are discussed as a possible cause of inflammation of the mammary gland during menopause. In addition, it was shown that women are affected by the hormonal conversion processes (Mastopathy) with the formation of small cavities filled with secretion (Cysts) in the breast tend to develop inflammation of the mammary glands more often, even during menopause. However, the exact causes have not yet been fully clarified.
Read more about this: Cyst in the chest
The symptoms correspond to those of the classic mammary inflammation. These are reddening, overheating and swelling of the affected area. In addition, the lesion is painful and the armpit lymph nodes on the same side may be swollen. Fever is rather atypical.
Inflammation of the nipple
The nipple is one of the most sensitive areas of our body and easily reacts to disruptive factors with inflammation. Often one can observe an involvement of the nipple with an inflammation of the mammary gland. As with mastitis, the cause can be blocked milk or an infection with bacteria. Other causative factors are allergies, tissue irritation during breastfeeding, breast malformations or new tissue formation.
It is important to note that inflammation of the nipple can also occur in men, mostly due to excessively rubbing clothing. The symptoms are similar to inflammation of the mammary gland with painful swelling and reddening of the nipple area. The armpit lymph nodes may be swollen on the affected side and a secretion may develop from the chest.
If the nipple is inflamed outside of breastfeeding in combination with a secretion, an examination should be arranged by a gynecologist as this can be an early sign of breast cancer. If there is no suspicion of a tumor, the diagnosis is made with a clinical examination analogous to mastitis.
Also read the article: The sebum glands of the nipple.
The therapeutic measures are also the same as for mastitis, although regular emptying of the breast during breastfeeding is only possible under severe conditions due to the severe pain. In addition, herbal ointments can be applied to the nipple, which can work directly at the site of inflammation.
Duration
In order to make a statement about the duration of the disease, a distinction must be made between inflammation of the mammary gland within and outside of breastfeeding.
During breastfeeding, mastitis can heal completely on its own or with local measures in a short time. Even if an antibiotic has to be taken, the symptoms usually subside within days.
In mastitis outside of breastfeeding, the symptoms also subside quickly when antibiotics or prolactin inhibitors are taken for non-bacterial causes. However, with this form of mastitis, the risk of recurrence, i.e. the risk that the mastitis will recur, is high, which is why great importance should be placed on long enough therapy.
In addition, a sufficiently long duration of therapy reduces the risk of chronic breast inflammation and the development of a breast abscess. Should an abscess develop in the course of the breast infection, this will extend the healing time. Since an abscess always has to be emptied by means of a puncture or a small skin incision, the duration of the wound healing is added to the regular duration of the disease, which can vary greatly from person to person.
When do you need antibiotics?
An antibiotic should be prescribed for any bacterial cause of mastitis. In the case of mastitis during breastfeeding, one first tries to influence the inflammation positively with local measures and emptying the breast for about 24-28 hours. However, if these measures do not lead to any improvement, an antibiotic should be prescribed quickly, as this is only effective in the early phases. Penicillinase-resistant penicillins or cephalosporins are given for treatment. Symptoms often improve rapidly with the use of antibiotics.
What are the effects of home remedies?
Home remedies are mainly used for local therapy. The cooling of the chest, which has an anti-inflammatory and pain-relieving effect, can be done, for example, with the help of quark compresses. Alternatively, ice packs, natural honey or acetic clay can be used. White cabbage leaves in the bra create even and long-lasting pleasant cooling. In addition, they also have a medicinal effect in that they have a positive influence on the milk congestion, which is often the cause of the inflammation.
In order to facilitate breastfeeding with mastitis during the lactation period, heat can be used. A hot shower or a red light lamp is ideal here.
To bring calm to the inflammation focus, a tight bra is recommended so that as little movement as possible affects the chest. In addition to the measures that act directly on the skin, home remedies can also reduce milk production. Drinking at least two cups of hibiscus, peppermint or sage tea a day can reduce the production of milk secretions.
Of course, care should be taken to ensure sufficient rest and fluid intake during acute inflammation in order to optimally support the body in combating inflammation.
In the case of inflammation of the mammary gland outside of breastfeeding, home remedies should at best be used to support drug therapy.
Homeopathy for breast inflammation
The homeopathic remedies used are used in breast inflammation in order to have a positive influence on the inflammatory process. Only a limited selection of possible means is described below.
In the early stages of the inflammation, belladonna or acidum nitricum can help. The latter especially with injuries to the skin in the form of small cracks. Bryonia is a good remedy for a swollen chest that causes severe and stabbing pain when shaken. Phytolacca or Pulsatilla are remedies that can be used well for mastitis during breastfeeding with radiation of pain in the shoulder and neck.
If the inflammation is at an advanced stage with the formation of pus, Hepar sulfuris can be used.
Read more about this: Homeopathic Medicines
Puerperal mastitis

Synonym: mastadenitis puerperalis, English: puerperal mastitis
Puerperal mastitis, which affects nursing mothers, is an acute inflammation of the breast that occurs two to four weeks after the birth (post partum) in the puerperium. It used to be the most common inflammation of the female breast. In recent years, however, their share of the total number of inflammations has decreased, whereas non-puerperal mastitis has increased.
Read more on the subject at: Breast pain while breastfeeding or puerperal mastitis
Origin and symptoms
Puerperal mastitis is an acute bacterial inflammation that in the vast majority of cases is caused by Staphylococcus aureus, a germ that can also be found on healthy skin. Also can Streptococci, E. coli, Klebsiella, Pneumococci and Proteus be involved, but this is less often the case. The germs can be Breastfeeding also to the mouth, nose and throat area Newborn be passed on. The nipples are mechanically stressed when breastfeeding. As a result, the finest cracks (rhagades) form through which the germs enter the lymphatic gaps of the Connective tissue of the chest reach. This is where the germs spread and accumulate.
Symptoms include classic signs of inflammation. The chest is reddened (Rubor), overheated (Calor), swollen (Tumor), in their Breastfeeding function restricted (Functio laesa) and hurts more or less strong (Dolor). The inflammation is usually limited to a restricted area, which is very often the case upper, outer area the chest (upper, outer quadrant). In addition, those affected generally feel weak and have fever. The Lymph nodes in the armpits can also hurt. While the inflammation is initially diffusely distributed in the chest, if treatment is neglected, a completed abscess result from it. Therapy is therefore essential.
Diagnostics and therapy
The clinical picture of mastitis is quite clear. By an additional Sonography an abscess can be displayed very well and precisely localized.
The therapy differs depending on the stage of the inflammation. in the Initial stage she is treated conservatively. Women should continue to breastfeed even if it was previously advised not to. There is practically no danger to the child. In addition, the chest is with Alcohol and quark wraps chilled. That works decongestant and pain reliever. However, alcohol compresses can dry out the skin. The chest is massaged and ultimately with it Antibiotics treated to kill the germs. The antibiotics that are used are Cephalosporins and Broad spectrum antibiotics. At an advanced stage, the therapy is somewhat different: if an abscess has already formed, the milk is pumped out and any further milk production is inhibited. For this one takes so-called Prolactin inhibitors. Lisuride, bromocriptine and cabergoline belong to this group of drugs. Prolactin inhibitors prevent the secretion of the hormone prolactin, which promotes milk secretion. There is a Heat therapy and finally one Abscess splitting. An abscess split is a surgical procedure to remove the abscess. Since scars always develop when an abscess is split, mastitis should be treated early to prevent it.
Non-puerperal mastitis
Synonym: Mastadenitis non-puerperalis, MNP; English: non-puerperal mastitis;
Non-puerperal mastitis can be bacterial as well as non-bacterial. It is an acute inflammation of the female mammary gland that is not associated with childbirth, pregnancy or the puerperium. MNP used to be considered a rather rare disease. It only made up about 5-10% of all breast infections. However, it now accounts for around 50% of the mastitis in sexually mature women. The reasons for this are not yet fully understood. There are diseases that are considered risk factors for developing MNP. These include inverted nipples, galactorrhea, macromastia, mastodynia, and a proliferating or fibrocystic mastopathy. In addition, the following factors increase the likelihood of developing non-puerperal mastitis: smoking, breast injuries, breastfeeding period that has elapsed, medication (tranquilizers, sex steroid preparations, ovulation inhibitors).
Origin and symptoms
- The bacterial MNP:
The most common pathogens of bacterial mastitis non-puerperalis are Staphylococcus aureus (40%) and Staphylococcus epidermidis (40%). Also E. coli, Fusobacteria, Streptococci and Proteus could be involved. However, this is less often the case. The bacterial MNP is favored by a Galactorrhea. That is the spontaneous exit of Breast milk (outside of the postpartum period). The MNP spreads in the milk ducts. A spread of the germs into the blood is rather rare. You can also Cysts ignite, e.g. as part of a Mastopathy.
- The abacterial MNP:
A non-bacterial mastitis non-puerperalis is caused by a increased secretion and thus by one Milk congestion caused. This increased secretion is usually due to one stress-related, hormonal or drug hyperprolactinemia traced back. The hormone prolactin promotes milk secretion. Hyperprolactinemia is the excessive release of this hormone that results in excessive milk secretion.As part of this, the milk ducts widen and the milk pours into the surrounding tissue (periductal tissue). In terms of a foreign body reaction, this leads to a inflammation. The inflammatory secretion can be rich in plasma cells (cells of the immune system), so that one can get a Plasma cell mastitis speaks.
The symptoms are similar to puerperal mastitis. An important difference, however, is that in non-puerperal mastitis the Body temperature is usually not increased. The Lymph nodes in the armpit are on the side of the inflamed chest in 50% of the cases swollen.
Diagnostics and therapy
Here, too, the clinical picture (the entirety of the symptoms) is clear. During the examination, it can be determined so quickly that it is mastitis. A Sonography be performed. In the case of non-puerperal mastitis, it is important to clarify whether it is a Malignancy (malignant tumor) could act. If the patient's condition does not improve despite therapy, a Mammography or one biopsy of the breast tissue.
The therapy is basically similar to that used for puerperal mastitis. It will come with Antibiotics treated (cephalosporins, oxacillin etc.). First and foremost, however, will Prolactin inhibitors used, especially in abacterial MNP. The prolactin inhibitors prevent further milk secretion so that the patients are usually symptom-free after two to four days. Should be a abscess have formed, this must be operated on. The chest should chilled and it is best to have a good grip Brassiere to wear.
Periductal mastitis
Periductal mastitis is abacterial non-puerperal mastitis.
More interesting information
Other topics that might interest you:
- Diseases of the female breast
- Puerperal mastitis
- Chest pain while breastfeeding
- Chest pain when ovulating
- Breast abscess
- Sebum glands of the nipple
- Breastfeeding
- Puerperium
- Breast cancer
- Galactorrhea
You can find an overview of all gynecological topics under: Gynecology A-Z