Hypokalemia
definition
Hypokalaemia is the condition when there is too little (Latin "hypo") potassium in the blood (Latin "-emia"). Potassium is a metal from the periodic table that is found in the blood along with some other metals.
Potassium is found everywhere in the body inside and outside of every cell and, together with sodium and calcium and other charged particles, forms an equilibrium which is often referred to only as the "salt balance" or "electrolyte balance". This balance ensures that every cell maintains an electrical voltage on its shell, its "membrane". This means that just by changing the amount of potassium (and sodium, calcium, etc.) processes such as muscle tension, digestion and any other tasks of the cells can take place.
If there is a fault in this equilibrium in the form of hypokalemia, this can have life-threatening consequences. The normal level of potassium in the blood is 3.6-5.2 mmol / L. Thus, values <3.6 mmol / L are referred to as hypokalaemia, values> 5.2 mmol / L are referred to as hyperkalemia.

Symptoms
Muscle cells are particularly sensitive to changes in potassium levels. If the potassium level in the blood serum falls, the electrical voltage that exists across the membrane of the muscle cells changes and the voltage drops. The cell becomes more difficult to excite. In the electrophysiological technical term, this process is called "hyperpolarization".
In the worst case, this leads to paralysis (Paresis) of the muscles. Conscious muscle movements are more difficult for those affected, bladder weakness and digestion weakened, which causes constipation. So-called "muscle reflexes" such as the Achilles or patellar tendon reflex are weakened.
The effects on the heart muscle are particularly acute and life-threatening. Initially, there are cardiac arrhythmias that can be detected by listening to the heart or recording an EKG. In severe hypokalemia, ventricular fibrillation can occur, in which acute defibrillation is necessary.
Read more about this under Recognize potassium deficiency.
Changes in the EKG
EKG is the abbreviation for electrocardiogram and is recorded to check the electrical activity of the heart muscle. With every heartbeat, the ions, the “metals”, are shifted between the inside and outside of the cells. This changes the electrical voltage that exists on every cell membrane and the cells are excited ("depolarized"), which leads to the contraction of the muscle fibers. The EKG measures the sum of all electrical voltages in the entire heart with the help of electrodes on the skin. This makes it possible to track how and in which direction the excitation in the heart spreads with each heartbeat.
With the EKG all consequences of hypokalaemia can be recognized. Starting with cardiac arrhythmias, through disturbances of the regression of excitation up to the life-threatening ventricular fibrillation, the doctor can follow all developments in the EKG. The signs of hypokalemia are T flats, ST depressions, U waves, and extrasystoles. However, these ECG signs can also occur without hypokalaemia and therefore do not automatically lead to the diagnosis of hypokalaemia.
The safest diagnostic method to detect hypokalaemia is to draw blood.
therapy
A permanent disturbance of the potassium level must be avoided at all costs. The imbalance not only represents a restriction in everyday life in many physical processes, but can also cause life-threatening situations in connection with cardiac excitation and cause lasting damage to the heart muscle.
The cause of the hypokalemia must be identified and corrected. There are several reasons for this, for example:
- Extreme malnutrition,
- Vomit,
- severe diarrhea.
However, hypokalemia can also be triggered with medication, for example in the context of insulin therapy or the use of diuretics, i.e., dehydrating drugs.
In the acute situation, regardless of the cause, the low potassium level must be corrected immediately. This is partly possible with food rich in potassium or potassium chloride tablets. In severe cases, potassium chloride must be given intravenously under close observation. An ECG should be run as a check in case hyperkalemia should occur.
causes
There are many different causes of hypokalemia.
First of all, gastrointestinal infections that lead to vomiting and diarrhea can lead to a considerable lack of potassium. Vomiting of other origins, such as bulimic disease, also has the same effect. In these situations the body loses a lot of salts and also stomach acid. This leads to a drop in pH. However, since the pH value has to be kept within a narrow range so that essential body functions can be carried out, a metabolic counter-regulation is switched on, which now begins to save acids. This happens in the kidney in exchange for potassium. Thus, more potassium is excreted, while H + atoms are reabsorbed.
Extreme malnutrition can also lead to potassium loss and deficiencies in all other minerals in the blood. This is simply because the intake is not sufficiently covered by the food.
However, hypokalemia can also be triggered by drugs.
Loop diuretics in particular, i.e. drugs that expel water and are used for pulmonary edema or heart failure, can cause increased potassium loss. These drugs inhibit the reuptake of various minerals, above all potassium, in the kidneys, so that these minerals are excreted in the urine.
But also insulin therapy for diabetes has the side effect of hypokalemia. Insulin ensures that the cells absorb sugar and potassium so that less potassium remains in the blood.
Also the so-called "Conn syndrome”Causes hypokalemia. This is what is known as primary hyperaldosteronism, which means that the hormone aldosterone is not subject to any feedback and is released in an uncontrolled manner. Aldosterone is responsible for the absorption of sodium in exchange for potassium in the kidneys. This means that an increased level of aldosterone is accompanied by a decreased level of potassium. There are three different causes of “Conn syndrome”: a hormone-producing adrenal tumor, an overactive adrenal cortex and genetic mutations. A sign of this syndrome is the noticeable hypokalemia at a young age.
Alkalosis
Hypokalaemia has metabolic effects on the organism. In particular, the electrolyte concentrations and the pH of the blood change.
If the potassium concentration in the blood is too low, the organism activates compensation mechanisms in order to stabilize the concentration, since the serum potassium must be kept in a narrow concentration range so that no cardiac arrhythmias occur.
The key organ for this compensation is the kidney. In the kidney, an exchange of potassium ions for hydrogen atoms takes place via specific exchange proteins. Potassium is absorbed, hydrogen atoms are excreted. The loss of hydrogen causes the pH of the blood to shift to the alkaline range, which means that it is below 7.35. Since this pH deviation does not correspond to the norm either, the lungs switch on as a compensation mechanism for the pH value: hypoventilation, i.e. a reduction in the breathing rate, takes place.
Cardiac arrhythmias
The potassium concentration in the blood is regulated within a narrow range: physiologically, it is between 3.6 and 5.2 mmol / l. This strict regulation is extremely important in order to avoid cardiac arrhythmias.
Both hyper- and hypokalaemia have an arrhythmogenic effect on the heart muscle cells. Hypokalaemia causes a decrease in the membrane potential of the heart muscle cells. This increases the risk of spontaneous arrhythmias. This can cause life-threatening cardiac arrhythmias, in the worst case ventricular fibrillation.
For this reason, the potassium level should also be checked regularly during drug therapy, especially when taking diuretics, and any deviations from the normal values should be urgently compensated for.
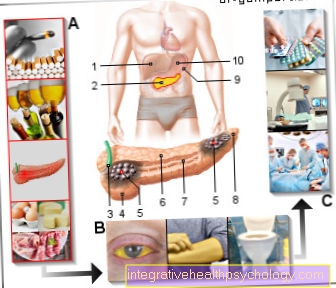
Insulin and its influence
Insulin is a hormone of the pancreas that is both produced and released with food intake and digestion and has a decisive influence on the sugar level in the blood. Insulin causes the cells to absorb sugar in the form of glucose, which is essential for their survival, and to transport potassium into the cell interior.
So insulin can significantly lower the potassium level. Thus, high insulin levels are a potential risk factor for hypokalaemia.
In medicine, this is used in the case of acute hyperkalemia, which can also be life-threatening. By administering glucose and insulin at the same time, one can lower the potassium level considerably. In doing so, however, attention must be paid to the correct dose so that it does not lead to fatal hypokalaemia.
Read more on the subject below Insulin - function & effect.













.jpg)