Lung abscess
introduction
A lung abscess is a circumscribed meltdown of lung tissue. Abscess cavities form, which almost always have purulent contents. There are different causes for this, mostly in connection with infections.

causes
Causes are mostly severe pneumonia, lung infarction, aspiration of purulent secretions (e.g. from a purulent tonsillitis), emphysema blisters, bronchiectasis, bronchial carcinoma with tumor disintegration, after an accident with accompanying spit or perforation of lung parts. In addition, abscesses that are located just below the diaphragm (subphrenic) and that spread through the diaphragm can lead to a lung abscess.
Spread of purulent infections via the blood or lymphatic system can also lead to this serious clinical picture. People who have a poor and weakened immune system are particularly at risk for lung abscesses. Particularly thin people, malnourished patients or tumor patients should be mentioned here. The spectrum of pathogens that leads to a lung abscess mostly consists of staphylococci or pneumococci.
For more information on lung abscesses, see the main abscess article.
Symptoms
A lung abscess can be completely symptom-free or be accompanied by severe symptoms of an infection.
The abscess itself, encapsulated by the pleura and the airways, can grow slowly and persist unhindered, but the symptoms are primarily triggered by the underlying cause. In most cases, it is caused by persistent pneumonia with the following symptoms:
- severe cough with sputum
- fever
- fatigue
- Chest pain
- Loss of appetite
- Shortness of breath
- Weight loss
- severely restricted general condition
The abscess can slowly grow towards the bronchi or pleura.
If it opens into these structures, it can suddenly lead to shortness of breath, coughing, severe pain when breathing and other symptoms. These symptoms are accompanied by strong bad breath. A new flare-up of the pneumonia, a pleural empyema, and bloody sputum can result. If the lung abscess persists over a long period of time without any concomitant disease, mild so-called B symptoms can draw attention to the disease. These include fatigue, paleness, weight loss, night sweats, and loss of appetite.
You may also be interested in this topic: What is the best way to prevent an abscess?
diagnosis
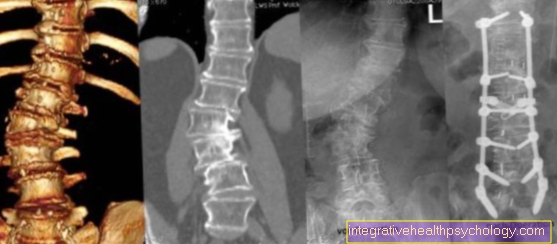
The diagnosis of a lung abscess can often be made based on the clinical picture. X-rays of the lungs are then conclusive. A computed tomography then shows the exact course of the abscess cavity. The blood count shows an increase in the inflammation values, such as CRP values, leukocytes and infection anemia. If lung abscesses have already been tunneled, bronchoscopy can show the abscess duct.
Pathogen
A lung abscess can develop as a result of a bacterial infection, such as pneumonia. The pathogen is detected by examining a blood sample or by diagnosing the sputum (sputum).
Typical pathogens that cause a lung abscess in pneumonia are pneumococci, streptococci, Pseudomonas, Legionella or Klebsiella.
Lung abscesses can also develop when bacteria from the mouth and throat are inhaled with the throat secretions and have multiplied in the lungs. These pathogens are mostly anaerobic bacteria that do not need oxygen for their growth, such as Becteroides, Peptostreptococci or Fusobacterium. Mixed infections with aerobic and anaerobic bacteria as well as an additional infestation with fungi or worms are possible with a lung abscess.
Computed tomography (CT) scan of the lungs
As an alternative to a chest X-ray, a CT image of the lungs can be made to diagnose or confirm the findings. With a CT, the lung tissue can be shown precisely and other diseases that also manifest as nodules in the lungs (e.g. tuberculosis or bronchial carcinoma) can be excluded.
therapy
Conservative treatment of lung abscesses consists of antibiotic treatment, as well as repeated bronchoscopic suction of the pus. A so-called vibration massage can also lead to an accelerated release of the secretion. If conservative therapy fails, surgical therapy usually has to be used, which consists of surgical opening of the abscess cavity and subsequent evacuation or suction. Then a wound drainage is inserted and the abscess cavity is rinsed regularly. Very large abscesses or chronic abscesses usually have to be completely surgically removed, which often means removing an entire section of the lung.
Antibiotic therapy
Lung abscesses are treated with antibiotic therapy. For this it is necessary to determine the pathogen by means of a microbiological examination of the blood or sputum (sputum). The antibiotics are chosen so that a broad spectrum of activity is covered and the treatment is effective against both aerobic bacteria (bacteria that require oxygen) and anaerobic bacteria (bacteria that can live without oxygen).
In most cases of a lung abscess, clindamycin is given in combination with cefotaxime or ciprofloxacin. Depending on the severity, so-called beta-lactam antibiotics such as ampicillin, piperacillin or amoxicillin can also be used to combat the pathogens. The antibiotic therapy takes place in the first few days via an infusion and then in the form of tablets. The entire treatment with antibiotics takes several weeks until the abscess has completely regressed.
Lung abscess surgery
A lung abscess is usually treated non-surgically, i.e. conservatively. Antibiotics are used here. In addition, a reflection of the bronchi (Bronchoscopy) carried out in which the Abscess cavity emptied and mostly one cytological specimen taken to prevent a malicious (malignant) Exclude process. As a rule, these two measures are sufficient to heal a lung abscess, even if the healing process extends over a longer period of time.
In rare cases, however, it can happen that a lung abscess cannot be healed with antibiotic and bronchoscopic therapy. The last resort is the operation in which the part of the lung in which the abscess is located has to be removed. As little lung tissue as possible is removed. Due to the size or location of the abscess, an entire lobe of the lung rarely has to be resected.
Complications
Complicated courses of a lung abscess consist of a permanent fistula formation (especially with chronic abscesses) and a breakthrough into the lung tissue. Severe cases can be septic, i.e. with life-threatening accompanying symptoms that can lead to death. Another serious complication is gangrene of the lung tissue, i.e. the death of entire sections of the lung. This mainly occurs when abscesses are discovered late and treated surgically or when abscesses recur in the lungs.
Pleural empyema
Pleural empyema is a collection of pus between the two leaves of the pleura.
The pleura consists of a sheet that directly envelops the lungs and a sheet that is attached to the inside of the chest. In this space there is a negative pressure as well as small amounts of a lubricating fluid to make it easier for the leaves to rub when breathing. In the course of pneumonia and a lung abscess, inflammation and involvement of the pleural leaves can occur. This can cause liquid pus to get between the pleural leaves and cause empyema, a type of pleural effusion. This can be very painful and make breathing difficult. Usually, the pus must be drained away until the inflammation subsides.
- Pleural Empyema - What's Behind It?
- pleurisy
Can a lung abscess be cured?
A lung abscess is basically curable and the lethality is low. How quickly or how well the abscess heals depends, in addition to the treatment method, primarily on the size of the inflammation focus and the number of abscesses.
Treatment is with antibiotics, with the development of antibiotic resistance being a possible complication. If antibiotic therapy does not work, drainage can also be used to empty the abscess. In severe cases it is also possible to remove part of the affected lung (segment resection or lobectomy).
Read more on the topic: Treating lung diseases surgically
forecast
Lung abscesses have a very different prognosis, depending on their cause, the underlying pathogen, the physical condition and the course of the disease.
If a small abscess occurs as a result of pneumonia in a person with healthy immune systems, the disease can usually be cured without any problems with a brief antibiotic therapy. Aggressive pathogens, large abscesses, immune deficiencies and concomitant diseases increase the risk of complications and dangerous courses.
Even if the abscess heals, permanent fistula formation in the lungs, sticking of the pleural leaves and damage to parts of the lung tissue can occur. Before this happens, a small part of the lungs can be surgically removed as a final therapeutic measure. Overall, the prognosis can be improved through timely and adequate therapy for pneumonia and its accompanying symptoms.
How can you distinguish a lung abscess from a lung tumor?
If a rounded structure in the area of the lung tissue is detected in the radiological image of the lungs, a tumor must always be excluded diagnostically, even if in most cases it is inflammation, abscesses or other lung diseases.
Important clues that indicate an abscess are accompanying or previous pneumonia. An existing fever and cough also initially speak for a lung abscess, even if these can also be symptoms of an advanced lung tumor. The most important means of distinguishing the two diseases is to determine the pathogen. First, an attempt is made to identify a pathogen in the sputum of the cough in the laboratory. A puncture of the abscess is also possible. In the laboratory, it can then easily be determined whether the infection is caused by the pathogen or tumor tissue.
Further information on this:
- How do you recognize lung cancer?
- Diagnosis of lung cancer