Mirena spiral
definition
The Mirena IUD is a hormonal IUD and therefore a contraceptive. The IUD is inserted into the uterus, where it constantly releases a hormone to prevent pregnancy. It is a so-called progestin, levonorgestrel, also called the corpus luteum hormone. The Mirena IUD is effective for about five years and is therefore one of the long-term contraceptive methods.

Effect of the Mirena spiral
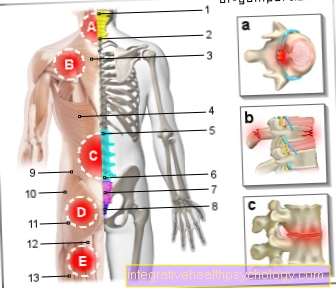
The Mirena spiral is a T-shaped plastic body. In its vertical part of the body this contains a cylinder filled with gestagens (levonorgestrel), which are similar to the body's own corpus luteum hormone. The IUD is inserted into the uterus by a gynecologist. Two plastic retrieval threads are attached to the spiral for later removal. They are palpable for the woman.
The coil works in the uterus through a local effect of the hormone levonorgestrel. This is dispensed evenly in small doses. At the start of contraception that is twenty micrograms in twenty-four hours and after five years only ten micrograms per twenty-four hours. The hormone is responsible for the contraceptive effect. It inhibits the build-up of the uterine lining and causes the mucus in the cervix to thicken. The thickened mucus prevents the sperm from entering the uterus.
Women who wear the IUD continue to ovulate. Pregnancy is prevented by the sperm and egg cells not being able to unite and implantation is prevented. In addition, the Mirena IUD has a positive effect on accompanying complaints during menstruation. In addition to contraception, it is also used for excessive menstrual bleeding (hypermennorhea) and for menopausal symptoms as part of hormone replacement therapy.
How safe is the Mirena IUD?
The Mirena IUD is one of the safest contraceptive methods and is used by around ten percent of all women of childbearing potential. Out of 100 women who use the Mirena IUD, less than one will get pregnant. This makes the IUD much safer than the pill and condoms. The only method of contraception that is even safer than the hormonal IUD is sterilization of the woman.
You can find a good summary on our website Overview of contraception methods
Mirena coil versus pill
The Mirena IUD and the pill are two contraceptive methods that work via hormones supplied with the contraceptive. While the pill, often consisting of a progestogen or an estrogen, prevents ovulation, the hormonal coil fends off pregnancy by making it difficult for the sperm to get to the egg cells and preventing the uterine lining from maturing necessary for pregnancy. Both ways lead to the prevention of pregnancy.
The pill is swallowed in the form of a small pill at the same time each day, while the hormone IUD remains in the uterus for about five years once inserted. Out of a hundred women who take the Mirena IUD, less than one woman becomes pregnant, while out of a hundred women who take the pill, eight women become pregnant. The IUD is therefore a much safer method of contraception than the pill.
Common side effects of the pill are headache and chest pain and occasionally symptoms such as dizziness, migraines, depressive mood, acne, hair loss and many more. Most of the side effects of both preparations are similar, but most of the side effects occur much more frequently with the IUD. At the same time, a hormonal coil can lead to puncture, perforation, the uterus, which is very dangerous. The two contraceptives are very different from each other and offer different benefits. A detailed discussion with the attending gynecologist is a good way of choosing the right contraceptive.
Cost of the spiral
The costs for the hormone IUD are not covered by the health insurance, they have to be paid by yourself. For the Mirena IUD, the costs are between € 138.08 and € 191.69, depending on the manufacturer and the package size.
More about this on our website What does the IUD cost?
Deployment costs
The costs for inserting the hormone IUD vary in gynecological practices. For the insertion and the necessary ultrasound examination, costs of 120 to 200 € arise. The costs for the IUD including its insertion are around 300 to 400 € in total.
That is how long the spiral works
Hormone IUDs work for three to five years, probably even longer, depending on the preparation. The Mirena IUD is a particularly long-acting preparation alongside the Kyleena IUD. It works safely as a contraceptive against pregnancy for five years.
This is how the Mirena IUD is used
The IUD is inserted by the gynecologist. This first examines the uterus, since the position, size and shape of the uterus are relevant in order to select the correct size of the hormonal coil. Typically, the IUD is used during the last few days of a menstrual period, as the cervix is soft and wide at this time. The gynecologist uses a tubular applicator to push the coil into the uterus. The security threads protrude from the cervix into the vagina even after the coil has been inserted. To relieve possible pain, the IUD can be used after administration of a pain reliever or under local anesthesia. The position of the hormone coil is checked with an ultrasound device and then checked every six months.
Read more about the use and the effect of the hormone and copper IUD under: The onset of the spiral
This is how the Mirena IUD is removed
The IUD is usually removed after five years, earlier if desired or in the event of complications. The gynecologist grabs the retrieval threads with special tweezers and pulls out the coil. As with the insertion of the IUD, pain medication or local anesthesia can be used beforehand.
Side effects of the Mirena IUD
The Mirena IUD can cause harmless to serious side effects. Common side effects of the Mirena IUD are headache, abdominal pain and pelvic pain and changes in menstrual bleeding from reduced to increased menstrual bleeding and even absence of the menstrual period. Other common side effects are inflammation of the vagina and vulva and vaginal discharge. In addition, depression, migraines, nausea, acne, a male hair growth pattern and back pain are often reported. Upper genital tract infections, ovarian cysts, menstrual pain, chest pain, and IUD expulsion are also common. Side effects that only occur occasionally are hair loss, discoloration of the skin of the face and neck, pregnancy spots (chloasma), hyperpigmentation of the skin and perforation of the uterus.
depression
In fact, depression and depressed mood are among the side effects that affect one to ten in 100 women. In order for the diagnosis of depression to be made, the symptoms must have been present for at least two weeks, otherwise one speaks of a depressed mood. The main complaints of those affected are a depressed mood, listlessness and loss of interest. Often the women also suffer from insomnia, loss of appetite, reduced attention and concentration and reduced self-esteem. Depression is a serious side effect of the IUD, so early removal should be considered.
possible complications
In addition to the mentioned side effects of the Mirena IUD, serious complications can occur. During the insertion of the IUD, the introducer may perforate the uterus. The insertion aid pierces the tissue and creates an opening in the abdominal cavity. Therefore, the position of the hormonal IUD is checked sonographically immediately after it has been inserted. If there is a perforation, surgical removal of the hormone coil and covering of the damaged tissue is necessary.
Another possible, rare complication is ectopic pregnancy. The fertilized egg embeds itself in the fallopian tube. Ectopic pregnancies do not allow the child to grow and are dangerous for women, so that an abortion must be carried out.
Drug interactions
There are hardly any interactions with other drugs to be expected, since the hormone coil acts locally in the uterus and releases hormones there. For the local contraceptive effect, it is irrelevant whether and which other drugs are taken. However, it is possible that the progestogens in the Mirena IUD are broken down more quickly if certain anti-seizure medications (anticonvulsants) and anti-infection medications are taken at the same time.
Does the Mirena IUD also work when taking an antibiotic?
The contraceptive protection of the Mirena IUD is not influenced by antibiotics. This means that the hormonal IUD has a preventive effect even when an antibiotic is taken. Each patient may have individual reasons that might speak against taking an antibiotic, such as an allergy. The attending physician should nonetheless be informed about the use of a hormonal IUD for contraception.