Oral thrush
definition
Oral thrush - also called candidiasis - is an infection of the mucous membrane of the oral cavity and throat with a certain type of fungus. In most cases it is the yeast Candida albicans.
However, this yeast is not disease-causing from the outset: normally, a small number of half of all people are found on the skin and mucous membranes and are not able to overcome the body's immune barrier and trigger an infection. Under certain circumstances, e.g. B. in a weakened immune system, however, they succeed in this, so that it comes clinically to a thrush. The disease can occur at any age. Oral thrush can also occur in the baby.
The term “thrush” comes from old German and means something like “to make sore” and thus describes the damage to the skin or mucous membrane caused by an existing fungal infection.
Also read the article on the topic: Changes in the mucous membrane of the mouth
causes

In most cases, the cause of oral thrush is an infection with the yeast Candida albicans.
However, one cannot actually speak of an “infection” in the actual sense: in almost half of all people, Candida albicans can be detected on the skin or the mucous membranes of the oropharynx or intestines without causing any symptoms.
Under physiological conditions, the yeast is not pathogenic enough to penetrate the defense barrier of the human body and trigger an infection, so that only superficial colonization takes place. Only under certain conditions, preferably whenever the immune system is weakened, does the fungus manage to multiply and trigger an infection (opportunistic infection).
Such defenses include both congenital and acquired immune disorders (e.g. in AIDS, cancer, under chemotherapy, in sepsis, diabetes mellitus, cortisone therapy or during pregnancy).
However, taking antibiotics can also cause oral thrush.
The antimicrobial effect can, in addition to the desired fight against bacteria, also destroy the physiological flora of the mucous membranes, so that the body's own bacteria also die. If these are significantly reduced in number, mushrooms, for example, have more space to multiply, so that over-colonization and infection can ultimately occur.
Among the actually healthy, infants and older people get (oral) thrush particularly often, which is due to the peculiarities of the immune system: in babies, the colonization with benign germs on the oral mucous membranes is not yet completely complete, so it is easier for the yeast to grow to multiply excessively.
In addition, there is the not yet fully developed immune system of the little ones, which means that the Candida fungus only has an inadequate defense against it. The latter also applies to older people, whose immune system is no longer as functional.
Read more on this topic at: How contagious are yeasts?
Oral thrush is caused by the colonization of the mouth with yeast. For this purpose, we recommend that you also read the following article: Yeast in the mouth
Medication as a cause of oral thrush
Certain medications can cause Candida albicans to overgrow. In the healthy oral flora there is a balance from different bacteria and fungi, which limit each other in their growth and thus ensure that there is no excessive growth of a specific species and thus a pathological infection. If bacteria are inhibited in their growth, for example by an antibiotic, and their numbers decrease, fungal spores can spread unhindered in the oropharynx and lead to oral thrush. At Immunosuppressants, i.e. drugs that inhibit the immune system, the result is an overgrowth with Candida albicans.
As well inhaled glucocorticoids, for example at bronchial asthma used can lead to an inhibition of the immune system. This effect is desired with regard to bronchial asthma, but at the same time also leads to the fact that the Candida pathogens are no longer sufficiently fought by the immune system and oral thrush can develop.
Cytostatics, so drugs that do that Inhibit cell growth, have also been linked to the development of oral thrush.
Also Antidepressants sometimes lead to oral thrush as a side effect. Depending on the type of action, they reduce the secretion of saliva and thus lead to one Dry mouththat favors the growth of Candida albicans.
Symptoms
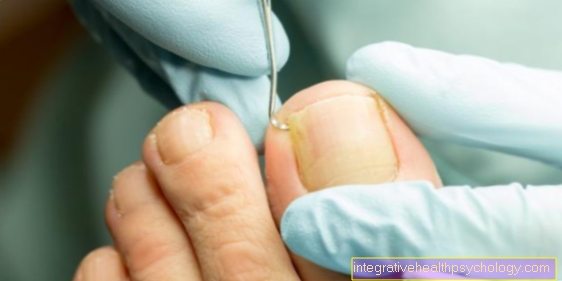
To the typical symptoms of oral thrush belongs primarily to the characteristic Appearance the mucous membranes in the oropharynx. On the strong reddened, inflammatory mucous membrane is a whitish coating that can be easily wiped off or scraped off, for example with a small wooden spatula.
At the beginning of the infection the coating is limited to more or less numerous whitish ones Stipple / sprinklel, preferably on the tongue, to him Inside cheek or on palate.
In the further course, the stipples can flow together (a so-called confluence), so that larger, whitish spots form. When such larger fungal coverings are removed, there may be slight bleeding of the underlying mucous membrane.
A predisposed infection site in the mouth is above all Dentures under which candida fungi can easily settle and trigger oral thrush.
In the case of more severe, complicated courses, in addition to the infection of the oral cavity, it can also spread to the Pharynx and / or the esophagus come (pseudomembranous candidiasis).
In addition, many sufferers complain of a dryness and furry feeling in the mouth and occasionally a burning sensation on the mucous membranes. In addition, taste disorders can occur, with a metallic taste perception being typical of oral thrush. Due to the feeling of dryness, many sufferers also notice an increased feeling of thirst, but a typical bad breath can also be observed.
diagnosis
Oral thrush can be diagnosed at first glance, usually by a doctor, based on its characteristic clinical picture.
The typical whitish coating On the tongue, the cheeks or in the throat there is hardly any room for confusion (except for the so-called Leukoplakia, one Tumor precursor).
If you are unsure whether it is a fungal infection or leukoplakia, a so-called Scratch attempt be undertaken: the whitish coatings of candidosis can be easily scraped off with a wooden spatula, whereas leukoplakia as tumorous changes in the mucous membrane cannot be scratched off or wiped off.
In order to be sure that it is a fungal infection and, above all, to determine the exact type of fungus, the treating doctor can ask you smear taken from the affected mucosa and placed in a laboratory in which the exact pathogen is diagnosed under the microscope.
In addition, antibodies against the Candida fungus can be found in the blood, but usually no blood draw is necessary as part of the diagnosis
therapy
The most common treatment for oral thrush is what is known as a doctor-prescribed treatment Antifungal agent. This is a medicinal product that either kills the fungi that are present or at least inhibits their growth or reproduction (this includes, for example, Nystatin, amphotericin B, fluconazole).
Since the oral thrush is a spatially limited infestation with Candida albicans it is usually sufficient to apply the antifungal agent locally, so that frequently on Lozenges, mouthwashes or direct sprinkling with a pipette is used.
If the oral thrush persists despite correct drug use or if other mucous membranes (e.g. in the gastrointestinal tract) are also affected, systemic control with antifungal tablets can also be considered.
infection
Strictly speaking, in most cases one cannot speak of an infection because, as already described above, Candida albicans is already present in the normal oral flora of some people, but is largely regulated by their immune system. However, certain behaviors can transmit Candida albicans to another person.
The mother, who already has candida on her, is often transmitted to an infant Oral mucosa, in your Gastrointestinal tract or on hers Vaginal mucosa wearing. A person who has a weakened immune system, or who is taking medication that inhibits the immune system or the production of saliva, is more likely to develop oral thrush. If this person now comes into contact with additional Candida pathogens via droplets or smear infections, these can no longer be sufficiently limited. Oral thrush breaks out.
Using the same toothbrush or the same cutlery also creates the risk of transmission.
Oral thrush in babies
Babies are not fully mature when they are born immune system. This leads to the fact that it is about up to 6 months of age in contact with Candida albicans the fungus can spread more widely.The ways of infection are varied.
In healthy adults, the fungus can be found in certain parts of the body without being noticed because the immune system fights it to the extent that it cannot spread. For example, some women have Candida albicans in their vagina without ever being affected. In the birth the newborn can become infected with this pathogen. Since, as already described, the immune system of a newborn is not yet fully functional, this often leads to oral thrush in the mouth and throat.
Also the nipple the mother is a possible source of infection for the infant, as the pathogens can also settle there. When breastfeeding, the pathogens are then absorbed from the mother's nipple into the baby's mouth. Itchy, themselves scaly or possibly also shiny red Nipples are often a sign of a candida nipple infection. It is also possible that the pathogen is unnoticed in the adult's mouth. If, for example, a fallen pacifier is put into the mouth by a parent to clean it, the pathogens can spread in the baby's mouth.
Another common cause of oral thrush in babies describes its poor hygiene. Toys, teething rings, or other things that babies put in their mouths can carry Candida albicans on their surface if they are not properly cleaned. Usually it is infection harmless. In babies, as in adults, oral thrush manifests itself with a characteristic white coating on the oral mucosa and tongue.
Additionally, oral thrush can cause a baby to have Poor drinking lead or easy fever trigger. For these reasons, a pediatrician should be consulted if suspected. Treating a baby with oral thrush is simple, but it can take until the infection has completely resolved 3 weeks last. In order to avoid the infection in advance, there are a few simple rules of conduct. For example, it is advisable to replace pacifiers that have fallen down and, in general, to thoroughly clean or sterilize things that the baby puts in its mouth.
An existing infection of the mother's vagina can also be combated before giving birth in order to avoid an infection during the birth.
Read more on this topic at: Oral thrush in babies