Patellar tendon irritation
definition
Patellar tendon irritation or patellar tip syndrome (tendinitis patellae or tendinosis patellae) is an inflammation of the patellar tendon.
The patellar tendon is the continuation of the anterior thigh muscle (M. quadriceps femoris). The task of the patellar tendon is to transmit force from the thigh to the lower leg, thereby allowing the leg to bend and straighten.
Overloading the tendon can irritate it and, in the worst case, even tear it completely.
Please also read the topic: Patellar tendon rupture

causes
Patellar tendon irritation typically results from continuous overloading of the extensor system in the leg. The increased friction at the junction between the tendon and bone causes irritation and the tendon becomes inflamed.
The patellar tendon is subject to strong tensile loads and constant stress, especially when walking and running. Therefore, runners who often and heavily strain their legs are often affected by patellar tendinitis. If you don't take enough breaks or use the wrong footwear, the development of patellar tendon irritation is further promoted. Good running shoes and sufficiently long breaks between runs are important preventive measures. Sports that often involve movements with many changes of direction, jumps or rapid braking (e.g. basketball, soccer, high jump, long jump, squash) are a major risk factor for patellar tendon irritation, as the tendon is extremely stressed and can be irritated quickly.
Another cause can be an insufficiently developed muscular system or a shortened thigh muscles, as this puts more stress on the tendon, rubs against the bone and can become inflamed. Patellar tendon irritation can also result from infectious wounds on the knee: as a result of an accident or injury, bacteria penetrate the tissue and trigger an inflammatory response there. Certain drugs, e.g. Statins (cholesterol-lowering drugs) or antibiotics from the class of fluoroquinolones also promote the development of patellar tendinitis, as they have a damaging effect on connective tissue and tendons.
Other causes and risk factors for the development of a patellar tendon irritation are various orthopedic changes to the musculoskeletal system, such as high knees, osteonecrosis of the patellar tendon or leg deformities such as knock knees and bow legs. In addition, being very overweight or age-related symptoms such as osteoporosis and arthrosis put a strain on the ligaments and promote inflammation in the knee area.
Symptoms
Typically, patellar tendon irritation is noticeable through pain in the kneecap, which is usually one-sided, but can also affect both sides. The pain usually increases with exertion, especially with exercise, climbing stairs, and walking downhill. The pain can also occur with everyday movements and can be triggered by tensing the anterior quadriceps muscle on the thigh. Depending on the extent and severity of the tendon damage, the knee can no longer be properly loaded and its function is limited, i.e. bending and stretching the leg is only possible to a limited extent or with pain.
Other symptoms are typical signs of inflammation: the affected knee swells, feels warm and the skin over it is reddened. As the tendon becomes damaged, the pain gets worse and in the worst case scenario, the patellar tendon can eventually tear. The knee then has to be operated on.
Appointment with a knee specialist?

I would be happy to advise you!
Who am I?
My name is dr. Nicolas Gumpert. I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
The knee joint is one of the joints with the greatest stress.
Therefore, the treatment of the knee joint (e.g. meniscus tear, cartilage damage, cruciate ligament damage, runner's knee, etc.) requires a lot of experience.
I treat a wide variety of knee diseases in a conservative way.
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You can find me in:
- Lumedis - your orthopedic surgeon
Kaiserstrasse 14
60311 Frankfurt am Main
Directly to the online appointment arrangement
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
Further information about myself can be found at Dr. Nicolas Gumpert
Pain
Patellar tendon irritation causes pain in the knee joint area. The pain can vary depending on the degree of inflammation. At the beginning the knee only hurts after exercise, e.g. Exercise or climbing stairs, later the pain also occurs during physical activity. As the inflammation increases, the pain persists, even if there is no stress.
diagnosis
If there is severe pain in the knee area, which increases with exertion, the suspicion of irritation of the patellar tendon is likely. A doctor can make the diagnosis by palpation and functional testing of the knee joint.
An examination is carried out for pressure pain on the patellar tendon and whether it is possible to stretch the leg against resistance. Imaging methods such as ultrasound or magnetic resonance imaging (MRI) are suitable for confirming the diagnosis. They provide information about how severely the patellar tendon is irritated and refine the prognosis.
Signs
Patellar tendinitis begins slowly and only slowly becomes noticeable. The first sign of an irritated patellar tendon is pain in the knee area between the shin and patella, which increases with exertion. Later, the pain can get worse and not only limit sports activities but also everyday movements.
What helps against patellar tendon irritation?
If the patellar tendon is irritated, anti-inflammatory agents called nonsteroidal anti-inflammatory drugs (NSAIDs), such as B. Ibuprofen, prescribed. The medication must be taken for several days, although taking it over a longer period of time is only allowed with a doctor's consultation. In the case of very severe inflammation or chronic cases, the doctor can use an ultrasound device to inject cortisone directly into the affected tendon. Cortisone has a strong anti-inflammatory effect, but the injections carry a certain risk, as they can make the tendon susceptible to tears. The use of pain relieving creams, such as diclofenac, is not particularly suitable for tendinitis, as the tendon is not supplied with blood and the active ingredient cannot penetrate well.
The most important measures in the event of patellar tendon irritation are protection of the knee, cold and heat therapy and regular exercises for mobilization. It is very important to keep the diseased knee still and to stop all activities that cause pain, otherwise the inflammation may become chronic or the tendon may tear.
Runners and athletes have to take a break and are only allowed to start training slowly again after the inflammation has subsided. If the inflammation is acute, the tendon should be cooled with ice packs and cold compresses to reduce swelling and redness. After a day or two, warmth helps the inflammation heal. Physiotherapy and physiotherapy support the healing process with targeted exercises for mobilization and stretching. Knee belts and knee supports relieve the tendon and thereby relieve pain. Kinesio taping also has a stabilizing and supporting effect on the knee joint.
Surgical intervention is very rarely necessary and is usually only used if the patellar tendon is torn.
Kinesio tapes
To relieve the pain and to accelerate the healing of a patellar tendon irritation, the affected knee can be fixed with kinesio tape. The elastic tape is stuck directly onto the skin of the thigh muscle and kneecap and supports the body's own healing process. Usually the tape stays on the diseased knee joint for four to seven days. The tape can either be applied by yourself or by a physiotherapist.
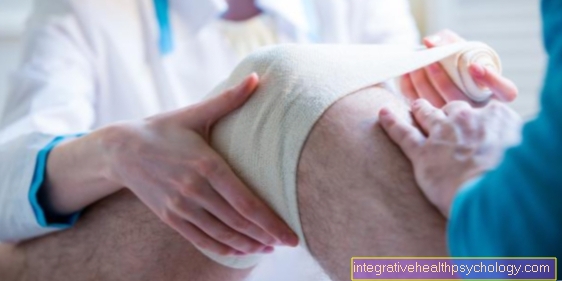
Bandages
An orthopedic bandage is prescribed by an orthopedic surgeon for treating patellar tendon irritation. It is important that the bandage is the right size, because it must not be too tight and cut or slip. The bandage stabilizes the knee joint and relieves the strain on the patellar tendon, allowing the inflammation to heal in peace without putting too much strain on the knee.
An example of such a bandage is the patellar tendon bandage.
stretch
Weak muscles make the patellar tendon even more tense and therefore have to withstand greater stress. Regular and constant stretching of the leg muscles promotes muscle building and thus reduces the strain on the patellar tendon. The stretching of the thigh muscles (front quadriceps, rear hamstring biceps) and the calves should not cause severe pain but only slight pulling. Even if the symptoms of patellar tendon irritation are gone, regular stretching can help prevent relapse.
Home remedies
Patellar tendon irritation is an uncomfortable condition that usually heals quickly. The best home remedy to speed up healing is as much rest as possible for the affected knee and a bandage for relief. In addition, the knee can be cooled for the first few days so that the swelling and pain subside. After two days at the latest, the inflamed tendon should be warmed with hot water bottles or infrared radiation so that healing is stimulated.
OP
Usually, irritation of the patellar tendon can be treated conventionally, i.e. without surgical measures.
However, in very rare cases, surgery can be considered as a therapeutic measure. This is especially the case with chronic and very long-lasting irritation of the patellar tendon. Due to the persistent inflammation, the tendon degenerates and shortens. During an operation, the damaged areas of the tendon are cut out and the tendon can regenerate.
psychotherapy
Supportive physical therapy may be prescribed to treat patellar tendon irritation. Massage techniques are used to stimulate blood flow. In addition, mobilization takes place through targeted stretching exercises, whereby the tension on the tendon is reduced and a normal sequence of movements should be achieved again.
Other exercises serve to strengthen the muscles in the thigh and calf. Physiotherapy usually lasts one to two weeks, after which the acute inflammation should subside and the knee should slowly be able to bear weight again.
Duration
Acute patellar tendon irritation usually heals on its own within a few weeks. The healing process can be accelerated through therapy and the entire illness then lasts about two weeks.
It is important that a period of at least two months is observed after the healing process in order to prevent possible relapses. In some cases, however, the patellar tendon irritation can become chronic and last for several years.
Sports break
During an acute patellar tendon irritation, excessive strain on the knee joint must be avoided and activities that cause pain should not be carried out under any circumstances. Even after it has healed, the tendon must be spared, otherwise relapses can quickly occur. Athletes, especially runners, are often affected by patellar tendon irritation.
You have to take a break from exercising until the acute pain has disappeared, as the patellar tendon is permanently stressed when you run.
You can then slowly begin again with the training, but you should make sure that the training units are short and not too demanding. Runners should choose short, flat stretches for the first few stretches after having overcome the patellar tendon irritation, if possible without curves or inclines.