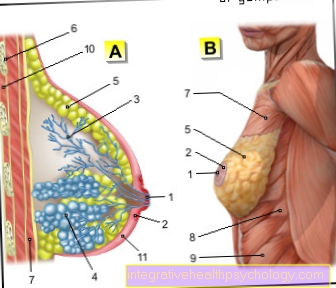
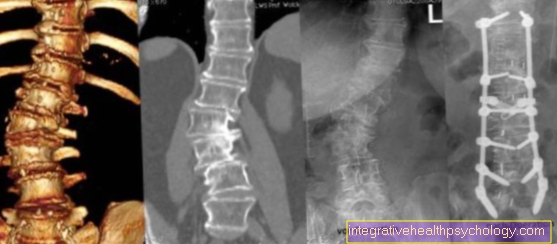
Symptoms of Cushing's Syndrome
Overview of typical symptoms
- Trunk obesity
- Moon face
- poor healing of skin defects
- Muscle loss (thin arms and legs compared to healthy people of the same age)
- Skin changes (thin parchment skin and a tendency to bruise)
- psychological changes (from mood swings to depression, often in children: aggressive behavior)
- Cloudiness of the lens of the eye (cataract = cataract)
- osteoporosis
- Weight gain
- increased susceptibility to infection

Often times, patients with Cushing's syndrome develop osteoporosis at a young age and complain of bone pain. Muscle weakness and muscle pain are also common symptoms of Cushing's syndrome. The patients feel powerless and lackluster. The following symptoms appear on the skin:
Wound healing in injuries is poor and the skin thins, which can be seen especially on the back of the hand. The patients also have red stretch marks on the skin (striae).
Also read the article: Cushing's disease.
Patients with hypercortisolism (too much cortisol) often develop diabetes mellitus, as cortisol causes sugar to be released into the bloodstream and thus high blood sugar levels can occur.
Cushing's patients have high blood pressure 85% of the time.
The development of depression is a not uncommon symptom in Cushing's syndrome.
Changes in the blood count can also be detected in Cushing's syndrome: the values for platelets and red blood cells and the total number of white blood cells are increased, while the values for special forms of white blood cells, eosinophils and lymphocytes, are decreased.
In women, symptoms such as menstrual irregularities and acne formation can occur with Cushing's syndrome. It can also lead to masculinization (androgenization). In 80% of cases, men with Cushing's syndrome have erectile dysfunction and there is a loss of libido in both sexes. When children have Cushing's syndrome, stunted growth and developmental delay occur.
Strong weight gain with "trunk obesity"
The strong weight gain during therapy with glucocorticoids is not necessarily due only to an increased accumulation of adipose tissue. The apparent weight gain is mainly explained by the visual change in the body caused by the glucocorticoids. Cortisone increases the breakdown of fat in the extremities at certain points. In addition, it ensures an increased breakdown of proteins, which manifests itself in muscle wasting. As a result, the volume of the arms and legs decreases, whereas the upper body often appears subjectively rather thicker than before. A “trunk obesity” is suggested. However, it is not necessarily increased fat that accumulates on the chest, stomach and back. Rather, it is water retention in the tissue that simulates weight gain. It is due to the additional effect of glucocorticoids on the electrolyte balance. An increased accumulation of fat is only found with a long-standing Cushing's syndrome due to an additional influence on the sugar metabolism.
Round "full moon face"
A round full moon face is a common symptom of Cushing's syndrome. The clear change in the shape of the face and the features of the face is in the foreground and is a psychological burden for those affected. The typical round face stands out next to clear cheekbones and a hinted double chin through reddened cheeks. The increase in volume is due to the side effects of glucocorticoids. In addition to their effect on the immune cells, they also have an effect on the electrolyte balance, which interacts with the water balance. The imbalance of the components ensures that more fluid is deposited in the tissue. The optical effect is a "puffy" looking face.
Muscle wasting: very thin arms and legs
Thin arms and legs are due to the metabolic side effects of glucocorticoids. They also influence the metabolism of proteins. Proteins are nothing more than proteins and are mainly found in muscle tissue. As a side effect, glucocorticoids increase the breakdown of proteins. Thus, as the therapy continues, muscle mass decreases until it shows up in thin arms and legs. However, glucocorticoids do not lead to a complete loss of muscle strength.
Muscle weakness
The muscle weakness in the context of Cushing's syndrome is due to the increased muscle breakdown during the therapy. Depending on the individual case, both the number of muscle cells can decrease and their cell structure can change. In precise terms, this means that existing muscle cells also deteriorate in their performance. Those affected notice this in a faster fatigue in stressful situations and possibly in a feeling of weakness. The drop in performance can vary depending on the previous level of training. Continuous physiotherapy or independent training sessions can have a positive effect on muscle loss. However, physical activities cannot completely avoid muscle wasting.
Read more on this topic at: Muscle weakness
Bone loss (osteoporosis)
The change in bone structure is a very late phenomenon in Cushing's syndrome. In addition, it is a symptom that its consequences are not always reversible by discontinuing the medication. The development of osteoporosis during glucocorticoid therapy is based on the influence on the filter function of the kidneys. Glucocorticoids act on the channels and transporters in the cell membranes of the kidney and thus lead to an increased excretion of calcium. Calcium is mobilized from the bone to compensate for the loss. Since the breakdown of the regeneration predominates, there is a loss of the healthy bone structure. However, it often takes years before skeletal abnormalities become apparent.
What might also interest you: Prevent osteoporosis
Bluish-red stripes on the trunk of the body, wider than 1 cm (stretch marks)
Bluish-red stripes on the trunk of the body are often found on the flanks and around the navel in Cushing's syndrome. This is because it is in these areas that the skin is usually the most stressed. It does not matter whether the load occurs as part of movements, touches or the laying of clothes on. In addition, these areas are predestined for an increased accumulation of fatty tissue, which additionally stresses the elasticity of the skin. If glucocorticoids are administered in higher doses, they cause permanent atrophy of the skin. So the elasticity of the skin decreases and both its structure and thickness change. This can be seen visually in bluish-red stripes, which are colored by the blood vessels located directly under the skin. A regression cannot be expected after the end of therapy.
Changes in the blood
Serious changes in the blood count are rather rare in the context of Cushing's syndrome. Rather, changes in laboratory values can be determined at the start of glucocorticoid therapy. Since it is usually applied due to an excessive immune reaction of the body with inflammatory symptoms, a significant reduction in the inflammation parameters can be observed. In individual cases and depending on the disease, a reduction in specific immune cells can be observed.
high blood pressure
It is entirely possible that high blood pressure will develop during therapy with cortisone. This is due to the effect of the glucocorticoids on the kidney. This is because they lead to an increased reabsorption of water and sodium in the organ. This means that less volume is excreted. It remains in the vascular system, where it leads to increased pressure on the vascular walls. Objectively, this phenomenon can be measured in elevated blood pressure values. How strong the expression of the high blood pressure is, however, depends on the individual case.
What might also interest you: Symptoms of high blood pressure
What is the Cushing's threshold for symptoms?
Long-term therapy with glucocorticoids should be less than 0.1 mg per kilogram of body weight in adults in order to avoid serious side effects such as Cushing's syndrome. Experts therefore speak of the so-called "Cushing threshold" for this dosage. If the administered dose is below this limit, however, isolated side effects can still be expected. A syndrome is then only very unlikely to develop.
You can find more information on this topic at: What is the Cushing Threshold?
masculinization
Masculinization is rarely seen in Cushing's syndrome. Those affected mainly complain about a loss of the typical female curves and the development of male body hair. The increase in male body features can be explained by an imbalance in steroid production. Steroid hormones are mineralocorticoids, glucocorticoids and sex hormones. All are made from the same starting substance - cholesterol. If an end product of the synthesis chain such as glucocorticoids is supplied to the body in the form of drugs, the synthesis rate of the other steroid hormones such as that of the sex hormones can be increased if necessary. Too much male hormones then manifests itself in masculinization.
Read more on this topic at: Androgenization - The masculinization
Stunted growth in children
Growth disorders in children can occur with long-term therapy with high-dose glucocorticoids. The growth is mainly due to the changed bone metabolism. Children's bones grow very quickly and need a lot of substrate in the form of minerals. However, glucocorticoids can cause more calcium to be excreted by the kidneys. This loss is compensated for by the mobilization of the body's own calcium from the bones. The bone structure loses its balance of cells and ingredients. A consequence of this can be delayed growth up to the development of bone deformities.
Read more on this topic at: Stunted growth in children
Mental changes
Mental changes are quite common side effects of glucocorticoids. However, it depends on the individual case how the effect on the psyche is expressed in detail. The most common development is from a depressed mood to manifest depression. However, a rather sad mood and a lack of drive do not always have to be in the foreground. In some cases it is also mood swings or mood swings that are particularly noticeable to relatives of the person concerned. A peculiarity in children is an excessively frequent aggressive behavior. It is not uncommon for the affected children to be noticed here because of their changed behavior at school.
What might also interest you: Signs of depression