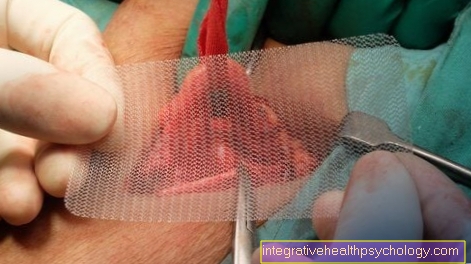
Therapy of a basalioma
How is basalioma treated?
There are several options for treating a basalioma.
The fact that basaliomas only have a low metastasis rate of 0.03% and thus "in principle do not form metastases" is of great importance for therapy planning (and that therefore only the one affected area of the body needs to be treated very locally).
However, they can still grow into the surrounding tissue and destroy it. Because of this, basaliomas are potentially very dangerous and should be removed as soon as possible. Which of the various removal methods is used depends on various factors such as:
- Age and general condition of the patient and
- Characteristics of the tumor such as its (location, growth form and extent)
dependent. In general, however, surgery is the therapy of choice because it has the greatest chance of success for a complete healing.
For more information, see the main page Basalioma.
Surgical removal of the basalioma

The therapy of first choice is the microscopically controlled surgical removal of the basalioma.
The operation of a basalioma can usually be done on an outpatient basis by a dermatologist, so the patient does not normally have to be admitted to a hospital as an inpatient.
Since the procedure is a rather small procedure, at least if the basalioma was detected at an early stage, it can usually take place under local anesthesia.
When excising the skin tumor, it is important not only to remove the tumor tissue, but also some of the surrounding tissue to ensure that it is completely free from the tumor and to reduce the risk of the tumor recurring (Relapse) to lower. During this procedure, the tumor tissue is excised sparingly, with a margin of 2-4mm. Often the edge of the cut out basalioma is viewed again under the microscope to see if there are still tumor cells in the edge.
If this is the case, a second operation is carried out in order to finally remove the tumor completely. If the basal cell carcinoma is very advanced and therefore has increased in size, surgical removal can sometimes lead to the formation of scars. Depending on the localization, these can lead to (mainly cosmetic) impairments, which is why another operation with a skin transplant is sometimes added.
Radiation therapy for a basalioma
Surgery for a basalioma is not always possible. This is the case, for example, when a surgical procedure is inoperable because of the proximity of the basalioma to other structures. Mostly it is a basalioma on the face or a basalioma that has remained undetected for a long time and that has grown far in depth. There are also other options for therapy.
The second choice is usually radiation therapy (Radiotherapy), as it can show results that are as good as an operation. However, its major disadvantage is that it has a multitude of side effects. In addition, one cannot examine the tissue for tumor cells and therefore cannot be sure whether the basalioma has actually completely disappeared.
This is why the recurrence rate is higher after radiation therapy than after surgery. Another advantage is the lack of damage to the skin, as there is no scarring and therefore better cosmetic results.
The standard technique here is irradiation with superficial X-rays. Depending on the size of the tumor, a safety margin of 0.5-1.5 cm is also maintained here. Organs at risk in the radiation field (e.g. eye, auricle, etc.) are protected with a lead cover.
The dose, i.e. the strength of the X-ray radiation, varies between 1.8-5 Gray, depending on the size and growth behavior of the tumor tissue. Radiation therapy usually requires several sessions.
Read more on the topic: radiotherapy
The icing therapy
Especially for elderly patients with smaller, superficial tumors, another method is freezing treatment (Cryotherapy) there. The tumor tissue is frozen with the help of liquid nitrogen at a temperature of -196 ° C and thereby destroyed, whereupon it is rejected by the body. Here, too, a safety margin should be observed. This variant is particularly suitable for tumors that are quite small and are superficial and close to sensitive structures, for example on the eyelid. A disadvantage of this therapy is that the icing sometimes causes skin changes on the affected area, which are on the one hand perceived as visually disturbing by many and on the other hand are often cause for concern because they are not clearly indicative of a tumor recurrence are different.
Photodynamic Therapy
For some years now, photodynamic therapy (PDT) has also been available for the treatment of basalioma. First, an ointment containing the active ingredient methyl-amino-oxo-pentanoate (MAOP) is applied to the affected skin area, which is then absorbed by the tumor cells. In these cells, the MAOP is converted into another substance, which is the target structure of the subsequent four hours of exposure to a special red light. Because the light is only absorbed by the cells that contain this specific substance, the energy released thereby selectively destroys only the tumor cells, but not the surrounding healthy tissue.
For detailed information on this topic, see: Cost of photodynamic therapy
Creams used to treat basal cell carcinoma

Local treatment with creams is also one of the newer therapy options. These contain either imiquimod or 5-fluoro-uracil as active ingredients. Imiquimod is a substance that stimulates the body's own immune system to attack tumor tissue as part of an inflammatory reaction. According to previous observations, this is a gentle method that does not lead to any residual symptoms and cures about 80% of those affected. However, since it has not been practiced for long, hardly anything can be said about long-term rates and a long-term risk of recurrences. 5-fluoro-uracil (5-FU) is a chemotherapeutic agent that is used systemically for various forms of cancer. Applied locally, it also causes an inflammatory reaction, which leads to the death of the tumor cells. In contrast to imiquimod, however, 5-FU is more aggressive towards healthy skin cells, which can change in an inflammatory manner through use. Both types of creams must be applied to the affected skin area for several (around 4 to 6) weeks, which can usually be done by the patient himself at home.
Read more on the topic: Imiquimod
Treatment with ointments
Local chemotherapy / immunotherapy should also be considered in the case of multiple basal cell carcinomas in several locations. Here, 5-Fuorouracil in the form of an ointment is given to the basaliomas daily over a period of approx. 4-6 weeks. 5-fluorouracil is a cytostatic, a drug that prevents tumor cells from growing. The cytostatic also induces an intended inflammatory reaction after 1-2 weeks. This is used to fight tumors by the own immune system. Another active ingredient that works in a similar way is imiquimod.
The disadvantage of therapy with cytostatic ointments is the frequent allergic skin reactions of the surrounding tissue. These inflammatory reactions, which arise through use, unsettle many patients, so that the patient often discontinues therapy early.
The chances of recovery from cytostatic therapy using local ointments are heavily dependent on the growth behavior and size of the basalioma.
Superficial basal cell carcinomas generally show a relatively high response to therapy.
Aldara
Imiquimod shows one in superficial basal cell carcinoma Healing chance of approx. 80%. It has an immune stabilizing effect and thus promotes the body's own immune reaction against the tumor tissue.
In practice, Imiquimod is known under the trade name Aldara®. In addition to basalioma therapy, it is also used for Treatment of warts used.
Relapse
Unfortunately, none of the therapy options can reliably protect the patient from the recurrence of the tumor, such Relapse forms at about 5 to 10% of those affected. It is therefore particularly important that patients see their dermatologist regularly after treatment Follow-up check present so that a relapse can be detected early and removed again if necessary.