Breast Cancer Subspecies
Synonyms in a broader sense
Breast cancer, breast cancer, invasive ductal breast cancer, invasive lobular breast cancer, inflammatory breast cancer, Paget's disease, carcinoma in situ
English: breast cancer

Is breast cancer the same as breast cancer?
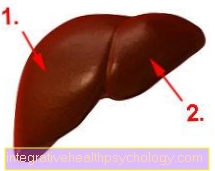
There are in principle many different types of breast cancer, depending on the cell type from which the cancer originally developed. However, some of these breast cancers are very rare and only play a minor role in practice. The two most important types of breast cancer arise from the cells of the milk ducts (ductules = lat. Duct) and the mammary gland lobes (lobules = lat. Lobules) and are therefore called "ductal" and "lobular" breast cancer.
Read more on the topic: How do you recognize breast cancer?
frequency
85-90% of breast cancer cases originate in the tissue of the milk ducts and are therefore ductal carcinomas. The decisive factor is whether the tumor grows within the milk ducts and their outer boundary - also known as the basement membrane - is intact or whether the tumor has grown beyond this boundary into the adjacent tissue. A further distinction is made here between non-invasively growing precancerous stages, also called carcinoma in situ, in which the outer border is intact, and invasively growing carcinomas in which the tumor has crossed the outer border. This distinction is important because it has an impact on the prognosis of breast cancer and the treatment options.
Lobular breast cancer is responsible for 10-15% of cancer cases. Here, too, a distinction is made between non-invasive and invasively growing tumors. If the tumor is confined to the tissue of the mammary glands, it is called a lobular carcinoma in situ; if it grows beyond the tissue, it is called an invasive lobular carcinoma.
For the structure of the breast see also our topic: Female breast
Breast cancer: classification
Classification of the WHO from 2001
A. Non-invasive tumors
- common carcinomas: ductal carcinoma in situ (DCIS), lobular carcinoma in situ (LCIS)
B. Invasive Breast Cancers
- common carcinomas: invasive ductal breast carcinoma, invasive lobular breast carcinoma
- Rare cancers: mucinous breast cancer, medullary breast cancer, papillary breast cancer, tubular breast cancer, apocrine breast cancer
C. Special forms
- Common carcinomas: Paget's disease of the nipple, inflammatory breast carcinoma
Carcinoma in situ
Under a Carcinoma in situ one understands a malignant tissue proliferation that does not grow invasively into the tissue. This means that its growth is limited to a superficial layer of tissue. It is therefore a preliminary stage of cancer that can still be treated surgically. If it is completely removed, it will no longer degenerate into an invasive form of cancer in most cases. However, if you leave a carcinoma in situ, there is a risk of degeneration, which, depending on the individual and the nature of the cancer, is only a matter of time.
The "DCIS" is sometimes also called the precancerous stage (Precancerous disease) designated. Since it has not yet broken through the basement membrane, no daughter tumors (metastases) can have formed. The transition time from DCIS to invasive ductal carcinoma is estimated to be less than ten years. Clear evidence that a finding is a carcinoma in situ can only be provided by the pathologist (examining the breast cancer tissue sample) after the entire suspicious area has been removed. Prior to this, none of the imaging procedures can rule out that the suspicious area has not broken through the basement membrane in a small area and thus developed into invasive (displacing) growth.
But even with the most careful examination of the tissue by the pathologist, the latter is not always able to provide reliable information about whether the basement membrane has remained intact. If the tumor extends more than 5 cm, the probability is approx. 60% that there has been an invasive growth through the basement membrane. Not every DCIS develops into an invasive form. It is assumed that around 50% of DCIS will later become invasive, but there is no reliable data on this. DCIS occurs independently in both breasts in 10-30% of cases.
Ductual carcinoma in situ is usually not palpable as a lump or hardening in the breast and the ultrasound usually does not show any of the findings. Most often, the DCIS is randomly diagnosed via mammography screening (see Sectie: Mammography) discovered. Scattered calcifications, so-called microcalcifications, which are often no larger than a millimeter in size, but appear bright white due to their composition, are particularly suspicious. However, this does not mean that a DCIS is hidden behind every calcification session in the mammography. Also, not every DCIS shows up through calcifications in the mammography.
Info: micro lime
The calcifications can be caused by dead cancer cells in a DCIS. These are then mostly located centrally in the tumor tissue, i.e. the extent of the cancer is greater than the area in which the calcifications are found. If microcalcifications were detected in the mammography screening, further images should follow specifically of this area. On the basis of the arrangement, extent and number of lessons and their form, it can then be decided in a next step whether it appears to be a benign change or whether further diagnostic steps should follow. Mammographically detectable microcalcifications are caused by carcinoma in around 20% of cases.
Van Nuys Prognostic Index
The Van Nuys Prognostic Index was created in order to be able to assess whether there is a risk of recurrence after the therapy has been carried out if a DCIS is present:
In this index, various properties are taken into account and evaluated with a point system, including the size of the area, degree of differentiation (grading) and width of the incision edge of the findings removed in the operation.
The degree of differentiation is assessed by a pathologist to whom the removed tissue is sent. If the cancer cells still resemble the tissue from which they arose, they are referred to as differentiated. The more the cells have changed, the less differentiated they are and the less favorable the prognosis. From the tissue sent in, the pathologist can also see how much space there is between the cancerous tissue and the cut edges in the healthy tissue. A greater distance is safer, but at the same time less gentle on healthy breast tissue. Each criterion (size, margin, grading) is classified with 1-3 points and added up so that values of at least 3 to max. 9, with 3 points representing the lowest risk of recurrence.
As an extension of the Van Nuys Prognostic Index, the patient's age is now also taken into account. Advanced age is favorable here for the prognosis. Based on the division into the Van Nuys Prognostic Index, the further therapeutic approach is also derived.
Van Nuys Prognostic Index
- 1 point
- Grading by the pathologist: Hardly any core changes and no necrosis
- Cutting edge in mm: more than 9
- Size of the tumor in mm: less than 16
- 2 points
- Grading by the pathologist: Hardly any core changes but necrosis
- Cutting edge in mm: 9-1
- Size of the tumor in mm: 16-40
- 3 points
- Grading by the pathologist: Strong core changes and necrosis
- Cutting edge in mm: less than 1
- Size of the tumor in mm: greater than 40
You can find more information on our website Breast cancer stages.
Special form of carcinoma in situ
A special form of DCIS is Paget's carcinoma, too Paget's disease of the nipple called. Is the DCIS near the nipple localized, it can spread to the skin of the nipple and cause inflammation with secretion and swelling there.
Not to be confused with Paget's disease of the nipple Paget's disease of the skeleton. It is a bone disease, the exact cause of which has not yet been clarified and which leads to bone remodeling and a higher risk of bone fractures.
Lobular carcinoma in situ
The lobular carcinoma in situ (LCIS) is relatively rare, it only accounts for 5% of all non-invasive tumors. It rarely leads to microcalcifications and is therefore usually found accidentally during a biopsy. In contrast to ductal carcinoma in situ, the LCIS itself is not assessed as a precancerous condition, but as an indicator of an increased risk (see also: Breast cancer risk) to develop breast cancer. LCIS occurs independently on both breasts at the same time in 40% of cases. There is no classification for the LCIS that is comparable to the Van Nuys Index.
What is invasive breast cancer?
Invasive breast cancer is a mass in the breast that infiltrates and displaces healthy breast tissue. It is therefore to be regarded as malicious. According to the depth of infiltration, a distinction is made between different stages of breast cancer, which, as it spreads, makes the cancer tissue more likely to spread to other organs. It is therefore characteristic that in its local growth it does not adhere to the natural boundaries of the breast tissue in relation to the lungs or other organs. It continues to grow and also affects tissue outside of its original organ.
Invasive ductal breast cancer
Invasive ductal cancer is the most common form of breast cancer at 70-80%. This also includes some rarer forms that differ in their prognosis and response to various forms of therapy. Invasive ductal breast cancer developed from cells in the milk ducts in the breast, but it has broken through the basement membrane that separates the ducts from other tissue. So it is no longer restricted to the milk ducts.
Invasive lobular breast cancer
Invasive lobular cancer, at 10-20%, is significantly less common than its ductal counterpart. It arises in the mammary gland lobes, but has broken through the separating basement membrane and has penetrated into other tissue.
The spread of this type of cancer is usually described as diffuse, which means that there are no clear boundaries to be seen. In addition, this type of cancer rarely forms microcalcifications, which means that invasive lobular breast cancer is mainly detected by MRIs of the breast or incidentally from biopsies performed for other reasons.
Invasive lobular cancer is rarely diagnosed using mammography.
Lobular breast cancer is not sensitive to radiation and is therefore treated differently from the ductal form.
Please also read our relevant topics:
- Breast cancer therapy
- Breast cancer chemotherapy
- Breast cancer radiation therapy
- Surgery for breast cancer
What is non-invasive breast cancer?
Non-invasive breast cancer can also be seen as a mass in the breast that does not, however, exceed the natural boundaries of the breast. This cancer, like invasive breast cancer, can be regarded as malignant, but does not destroy the body's own breast tissue. Rather, it displaces other tissue through its increasing volume than infiltrating it. This form of cancer also has the ability to spread, but it is more or less likely depending on the exact type of breast cancer.
Inflammatory breast cancer
Inflammatory breast cancer is extremely rare, accounting for around 1 to 4% of all breast cancer cases. This leads to diffuse cancer cell growth along the lymphatic vessels of the skin. Symptoms that occur are e.g. redness, overheating or an orange peel phenomenon (see also: Breast cancer detection). Inflammatory breast cancer often resembles a breast inflammation (mastitis). In contrast to mastitis, the patient does not experience any pain or fever.
Overall, inflammatory breast cancer has a very poor prognosis.
Paget's disease
Paget's disease (also called Paget's carcinoma) is a form of breast cancer that predominantly arises from ductal carcinoma and affects the nipple, and sometimes the entire areola as well. The tumor usually occurs on one side and can initially be mistaken for an inflammatory change in the nipple. However, this usually occurs on both sides. In more advanced stages, the tissue-damaging growth of the cancer can lead to a retraction of the nipple.
Read more about it on our page: Paget's Disease.
Receptor status
The pathologist examines a removed tissue sample not only for the type of cancer and the appearance of the cells. With certain staining and measuring techniques, the hormone receptor status is also routinely ascertained if a breast cancer lump is present.
Scientists have been able to show in the past that many breast tumors have receptors to which the female sex hormones estrogen and progesterone can dock and thus stimulate cancer cells to grow.
Another type of receptor that is routinely checked is the HER2 / neu receptor. It is found on the surface of healthy breast cells, but also on most breast cancer cells. The HER2 / neu receptor belongs to a class called growth factor receptors. If it is activated, it leads to the development and growth of the cell. How many HER2 / neu receptors a cell has is determined by a specific gene in the cell. In tumor cells, this gene is often more frequently found as a copy and there can be a 10-100 times higher number of receptors. This stimulates the cancer cells to grow more easily and more strongly than healthy cells. There is also a scale for the HER / 2neu receptor that ranges from 0-3, where 0 means that there is a normal number of receptors.
Please also read our page Tumor markers in breast cancer.
Do you need detailed information on this topic?
At this point we would like to point out that a detailed book has been written on this subject.
Learn to better assess the chances of recovery, conservative and operative measures, as well as the risks. Learn how to properly deal with the disease of breast cancer and become a competent discussion partner for your doctor.
Hormone receptor status
Evidence of Estrogen receptors (ER +) or Progesterone receptors (PR +) is important for further therapy and prognosis. For those tumors that have receptors, the possibility of hormone therapy offers itself. By changing the hormone balance in a certain way, there is then the chance to prevent the formation of metastases and to slow down the further growth of the tumor. 2/3 of all breast cancer tumors are receptor-positive, but they differ in the number of receptors.
A scale from 0-12 indicates how many receptors a cell of the removed tissue has, where 0 stands for nonexistent (negative for the receptor). The number of receptors depends on the response to anti-hormone therapy: a higher value on the scale means an increase in the effectiveness of the therapy that can be assumed.
Women before Menopause more often have receptor-negative tumors, women after the menopause are more likely to have receptor-positive tumors. See under therapy: anti-hormone therapy.
estrogen
New breast cancer therapies are based on the receptor status of the respective tumor. For this purpose, samples are taken from the mass in the chest in advance and carefully examined for their condition. With knowledge of the exact tumor characteristics, a targeted therapy can then be started that destroys the cancer as precisely as possible and at the same time minimizes side effects. Many breast cancers are positive for the estrogen receptor. This means that this tumor grows faster under the influence of estrogen. If this receptor is now blocked, the cancer is deliberately inhibited in its growth.
progesterone
Another typical receptor in breast cancer is the progesterone receptor. Just like with the estrogen receptor, a positive test result means that the hormone progesterone allows breast cancer to spread faster. In other words, its growth is accelerated by the sex hormone. If this receptor is blocked, the cancer will be treated in a targeted manner.
HER1
HER is the abbreviation for "Human epidermal growth factor receptor“And actually describes itself very well. In fact, these are growth factor receptors on cancer cells that, when activated, support the growth of the cancer. Seen figuratively, one can imagine it as a switch which - if it is tipped over - leads to an initiation of growth processes. HER1 just means that there are several of these subtypes of receptors and that they are therefore simply numbered consecutively. If breast cancer is positive for this receptor, the blockade of the receptor also represents a targeted therapy against the cancer.
HER2
As already mentioned, HER2 is just another subtype of growth factor receptors. It is important to know that breast cancer does not have to be HER1 and therefore HER2 positive at the same time, but that both types of receptors can occur independently of one another in breast cancer. There are effective therapies for both variants that can be designed, among other things, with the administration of antibodies. These antibodies then block the signal at the receptor and the breast cancer is prevented from spreading.
Read more on the subject at: Antibody Therapy (Anka)
Triple negative
Triple negative is a type of breast cancer that is negative for all three of the aforementioned receptors. This means that exactly this breast cancer is not positive for estrogen, progesterone or HER1 / HER2. Its growth is therefore completely independent of these hormones and receptors. This type of breast cancer is therefore more difficult to treat than others, as no precise cancer structures can be attacked or blocked. In most cases, high-dose chemotherapy must then be started with possibly combined radiation, which destroys other healthy body tissue in addition to the cancerous tissue. So the side effects are greater in this case.
This article might also interest you: Side effects of chemotherapy for breast cancer
What are the chances of a cure for each type of breast cancer?
It is difficult to predict the chances of a cure specifically for each type of breast cancer, because ultimately the interplay of many factors is decisive for the prognosis of breast cancer. A distinction is made between so-called favorable and unfavorable factors that are directly related to the disease. Apart from the type of breast cancer, the condition of the patient also plays a major role. Other previous illnesses worsen the chances of recovery from breast cancer, whereas an otherwise good general condition has a positive effect. The 5-year survival rate for women with breast cancer is about 88%. This means that 88 out of 100 women diagnosed with breast cancer are still alive after 5 years. For men, the survival rate is slightly worse at 76%. That's because men often have more aggressive types of breast cancers than women.
There are no precise data on the chances of a cure or survival rates of individual breast cancer types, but factors can be narrowed down that improve or worsen the chances of a cure. A distinction is made between three risk groups, which are also very important for the therapy decision. The first group - low-risk breast cancer - includes tumors that have a better chance of recovery than other types of breast cancer. For breast cancer to belong to the low-risk category, certain criteria must be met. Lymph nodes must not be affected and the tumor size must be less than 2 cm. The involvement of lymph nodes is always to be seen as unfavorable and worsens the chances of recovery. Furthermore, no vessels must be affected, as there is then the risk of rapid metastasis - i.e. spread of the cancer.
A patient age over 35 is considered favorable. Younger women with breast cancer are usually carriers of a certain gene mutation (BRCA1 or BRCA2 mutation) that can lead to various cancers at an early age. Furthermore, the degree of degeneration ("grading“) Of the tumor plays an important role. Tumors that the low risk group are assigned the degree of degeneracy G1. This means that the cells of the tumor are still very similar to the original tissue. The higher the degree of degeneration of the tumor, the worse its chances of recovery.
For some years now, breast cancer has been checked for its so-called hormone receptor status. Tumors with many hormone receptors have a better chance of recovery because they respond well to therapy with certain drugs. However, one particular receptor, the Her2 receptor, has an adverse effect on survival. Tumors that have the Her2 receptor are more aggressive than those that are negative for this receptor. Apart from the low risk group also exist one intermediate- and a high risk group. The latter show rather poor chances of recovery and are characterized by lymph node involvement or other unfavorable factors, such as the lack of hormone receptors or the presence of the Her2 receptor. The healing tendency of breast cancer is a very individual matter and results from the interplay of many factors. Therefore, it cannot be given across the board for each type of breast cancer. However, one can differentiate between favorable and unfavorable constellations.
These articles might also interest you:
- Chances of recovery in breast cancer
- Prognosis in breast cancer
- The breast cancer gene
TNM for breast cancer
The TNM classification is divided into three areas, with the “T” standing for the size of the tumor, the “N” for the number of affected lymph nodes and “M” for distant metastases. The exact information in each category allows a good prognosis and at the same time determines the therapy options. A small tumor that has not yet spread is primarily operated on and thus has a good chance of recovery. A large tumor, on the other hand, may have to be irradiated first so that it loses volume and then operated on. From a medical point of view, the information about the breast cancer must be much more precise, so that the size of the tumor is divided into T1 (5 cm) and T4 (any breast cancer that affects the chest wall or skin). The number of affected lymph nodes is also specified more specifically by also naming the exact region (armpit, collarbone, etc.). The final classification then results in an individual scheme for each patient that always serves as a reference for the course of therapy. Improvements or deteriorations can therefore be objectified from a medical point of view. But this classification also offers some patients the opportunity to better understand their illness and to get a rough idea of the extent of it.
What is the prognosis?
The prognosis of individual breast cancer types results from the interplay of many important factors. It can therefore not be given across the board. In addition to the type of breast cancer, the lymph node involvement plays an important role. Basically, the involvement of the lymph nodes in the armpit is the most important prognostic factor. From there, breast tumors form metastases in other organs, which greatly impairs survival. An unfavorable prognostic factor is the presence of the Her2 receptor on the surface of the tumor. Such breast cancers tend to behave aggressively, which is why their prognosis is worse compared to tumors without the Her2 receptor. The most unfavorable prognostic factor is a negative hormone receptor status of breast cancer. This means that there are no receptors for hormones like estrogen or progesterone. This eliminates the possibility of therapy with drugs that target these receptors. Therefore, the prognosis for such tumors is rather poor.
Further information on the topic can be found here: Prognosis in breast cancer
Classification of breast cancer
G1
The “G” in the classification of breast cancer stands for “grading” and describes nothing other than the cells from a sample of the tumor. A pathologist uses defined cell characteristics to assess how malignant the cells look and classifies them from well differentiated to poorly differentiated. Differentiation means how similar the cells look to the actual cells of the original tissue or, simply put, whether they still have a similarity to healthy body cells. The more they resemble the body's own cells, the better the prognosis. G1 means that it is a well-differentiated cancer. The prognosis can therefore be assessed as good from a histological point of view.
G2
G2 means that the cancer cells from the sample are less similar to the actual body's own cells. The degeneration of the tissue is therefore more pronounced than in stage G1. In technical terminology, G2 is described as moderately differentiated. A typical characteristic here is, for example, the shape and size of the cell nuclei, which deviate more clearly from the norm than in G1.
G3
G3 is a poorly differentiated tumor. The cells no longer have any resemblance to the original cells in the breast tissue. This usually means that this cancer is very aggressive and spreads quickly. The prognosis is accordingly worse than for the other G stages. For therapy, this means maintaining sufficient safety margins during operations and subsequent chemotherapy or radiation if necessary.
This article might also interest you: Irradiation for breast cancer
What are aggressive breast cancers?
Some types of breast cancer are classified as aggressive because they either respond poorly to therapy or have a tendency to metastasize after a short time. The exact classification of breast cancer types is very complicated and is based on various prognostically relevant factors. Therefore, general statements should only be made very carefully. Above all, tumors that show a high degree of degeneration ("grading") exhibit. This means that the cells of the tumor hardly look like the original tissue from which they arose. Such tumors are classified as G3 or G4. An example of such an aggressive tumor is poorly differentiated, invasive, ductal carcinoma, which has a degree of degeneration of G3 or G4.
However, other types of tumors can also be considered aggressive if they show a high degree of degeneration or other prognostically unfavorable factors. An important criterion is the Her2 status of the tumor. Breast cancers that are positive for the Her2 receptor behave more aggressively than those that are negative for this receptor. This is another example of a more aggressive breast cancer inflammatory breast cancer This tumor tends to quickly metastasize and invade the lymphatic vessels of the skin. Mostly ductal tumors are involved, but lobular carcinomas are also possible. The inflammatory breast cancer shows a 5-year survival rate below 5% if left untreated. Even with optimal therapy, only every second woman is still alive after 5 years.