The femoral neck
definition
The femoral neck is a section of the thigh bone (os femoris, femur).
The femur can be divided into a total of four sections. The femoral neck (collum femoris) follows the femoral head (caput femoris). This finally goes into the thigh shaft (corpus femoris). Finally, the thigh bone has two bony protrusions (condyli femoris) at knee level, which are involved in the structure of the knee joint. The femoral neck itself lies for the most part in the joint cavity of the hip joint and is surrounded by the joint capsule.
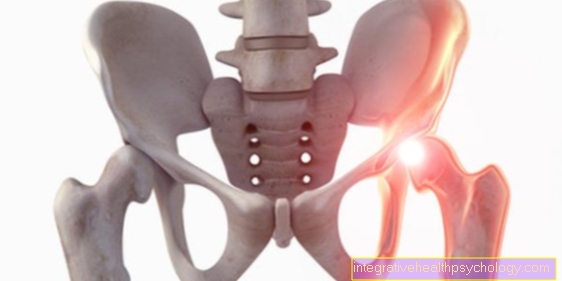
anatomy
Anatomically, the thigh neck (collum femoris) is a part of the thigh bone (os femoris, femur). It represents the connection between the femoral head (caput femoris) and the thigh shaft (corpus femoris).
The thigh neck is angled towards the thigh shaft towards the center of the body. This angle is called the CCD angle (caput-collum-diaphyseal angle) and is approximately 126 °. If the angle exceeds this value by about 10 °, one speaks of a coxa valga, if it is smaller than 120 °, it is a coxa vara.
The femoral neck merges into the femoral shaft. Two anatomical structures are noticeable at this transition. The greater trochanter and lesser trochanter are two bony protrusions from which various muscles originate.
In addition, the thigh neck is involved in the development of the hip joint. Two thirds of it is surrounded by a joint capsule, but it is not involved in the direct mechanics of the hip joint. Nevertheless, it is completely surrounded by the so-called synovial membrane, which ensures the nutrition of the joint and the smooth movement of the femoral head in the joint socket.
Some blood vessels (collum vessels) that supply the femoral head also run directly on the femoral neck. Furthermore, the thigh neck is covered by a strong ligament, which secures the hip joint and makes it less prone to contortions (dislocations).
Muscles on the thigh neck
Different muscles have their attachment point at the thigh neck or at the transition to the thigh shaft.
A powerful hip flexor is the iliopsoas muscle. It is made up of two muscles (iliacus and psoas muscles), which together form one muscle. Among other things, it begins on the lumbar vertebrae and runs through the inguinal ligament. Its starting point is the lesser trochanter, a small protrusion of bone at the transition from the femoral neck to the femoral shaft. Its movements are both hip flexion and internal rotation (inward rotation of the thigh). It is supplied by the femoral nerve, which comes from the spinal cord segments Th12-L4.
The gluteus medius and minimus muscles are attached to the greater trochanter, a larger protrusion of bone on the thigh neck. Its main function is to abduce the leg. In addition, they are also involved in flexion, extension, internal and external rotation (inward and outward rotation) of the hip.These two muscles are supplied by the superior gluteus nerve from the spinal cord segments L4-S1.
The piriformis muscle, a smaller muscle under the gluteal muscles, also attaches to the greater trochanter and supports abduction.
Read more about thigh muscles at: Thigh muscles
How can you properly stretch the muscles in the thigh neck?
On the thigh neck you can stretch both the large hip flexor muscle (Musculus iliopsoas) and the small gluteal muscles (Musculus gluteus medius and minimus).
There are several exercises to properly stretch the iliopsoas large hip flexor muscle. During a stretching exercise, the patient stands in a step position and pushes the hips forward. A slight stretch should be felt in the back leg.
Another variation of this exercise is kneeling. Here, too, care should be taken to push the hips far forward and keep the knees parallel. Both positions should be held three times for 20 seconds each.
The gluteus muscles can also be stretched in different ways. An exercise can be done while sitting. To do this, the patient sits upright on a chair and hits the leg to be stretched on the other. Here you put the ankle of the leg to be stretched on the knee and unfold the leg. This external rotation can be increased by pressing so that you feel a pull in the buttocks area. One way to increase the stretch is to lift the heel of the raised leg. This exercise should also be repeated three times and held for 20 seconds each time.
Diseases of the femur neck
Femoral neck fracture
Femoral neck fractures are fractures in the area of the femoral neck (collum femoris) and lie between the femoral head (caput femoris) and the trochanters (protruding bones at the transition to the femoral shaft).
The fractures are divided into medial intracapsular and lateral extracapsular femoral neck fractures. The course of the fault line is decisive for a healing prognosis. According to Pauwels, this can be divided into three prognostically important degrees of severity.
In Pauwels I, the break lines run up to 30 ° to the horizontal and there is a favorable prognosis for healing.
Pauwels II extends up to 50 ° and Pauwels III describes all fault lines over 50 °. In this case, there is a risk of high-grade hip instability in the future. The fracture itself is also divided into four degrees of severity. This division was named after Garden, which describes the degree of dislocation of the break. Garden I describes an incomplete fracture, whereas Garden IV characterizes a complete fracture. Here the fracture surfaces are shifted from one another and have no contact with one another.
If a patient is diagnosed with a femoral neck fracture according to Pauwels I and Garden I, physiotherapy is sufficient for healing. All other degrees of severity must be treated surgically.
Please also read our main article on the subject: Femoral neck fracture
What is the mortality rate for a femoral neck fracture?
The femoral neck fracture is a fracture that occurs particularly in the elderly over 65 years of age. The reasons for this are that older people fall more often, for example because they have poor eyesight or react more slowly. In addition, people over 65 years of age have weaker bones and are therefore more prone to fractures.
With a femoral neck fracture, the mortality rate is quite high, although the operation in itself is a minor complication. The long recovery period following the surgical procedure is more problematic. The often older patients are bedridden for several weeks and thus run the risk of dying from a secondary illness. Particularly noteworthy are pneumonia, severe inflammation of the wound or thrombosis.
The best therapy, however, is to mobilize the patient as early as possible. It is extremely important that patients become active and move again during the long healing process (at least 12 weeks). Although this has improved over the past few years, a third of patients still do not fully recover from the operation and even have to be placed in nursing homes.
Transient osteoporosis of the femoral neck
Transient femoral neck osteoporosis is a temporary disease of the hip.
In this case, if the cause is unexplained (idiopathic), bone substance in the area of the femoral head and femoral neck often dissolves. Patients experience increasing pain with exertion and while walking. A limping gait is also noticeable.
An early diagnosis is often difficult to make, since bone loss of over 40% is noticeable on X-rays. This disease is increasingly affecting middle-aged men and is also known as bone marrow edema syndrome (BMES).
Thigh neck pain
Femoral neck pain is a non-specific symptom and can have various causes.
For one, it could be a problem with the femur itself, such as a fracture or bruise. On the other hand, the hip joint can be dislocated (luxated) and it must be returned to the correct position. Furthermore, an inflammatory process can also be the cause of the pain, e.g. an inflammation of the bursa. A muscular cause must also be considered. Often there is a shortening of the large hip flexor iliopsoas due to too long sitting and too little movement. Due to this variety of causes, it is advisable to consult a specialist.
Read more on this topic at: Hip Bursitis - How Dangerous Is It?
Inflammation of the thigh neck
Inflammation can occur in the thigh neck, which is manifested by several symptoms. Patients often describe tenderness on the outside of the hip that is aggravated by walking. Inflammation of the bursa (bursitis) or inflammation of the tendons (trochanteric endinosis) that run over the greater trochanter come into question. Several tendons of various muscles, which are heavily used, run over the large roll mound (greater trochanter). Thus, increased irritation is not uncommon at this point.
The diseases are treated with medication, physiotherapy, heat or cold therapies and shock wave treatments. In the case of chronic inflammation, surgery can also be useful.
You can also read about this:
- Tendinitis of the thigh,
- Hip Bursitis - How Dangerous Is It?
Bursitis
Bursa are embedded in protruding bones to protect skin, tendons and muscles. In the event of long-term and excessive exposure, these can ignite. A typical spot for such an inflammation of the bursitis (bursitis) is the so-called large roll hillock (greater trochanter) on the thigh bone.
An inflammatory reaction occurs and the patient suffers from swelling and tenderness. First, conservative therapy is given with an anti-inflammatory pain reliever. In addition, the patient should take it easy and avoid physical strain. Placing cold packs on the skin can also bring relief. If these measures do not help, the bursa must be surgically removed.
Read the article on this: Bursitis surgery
Cyst in the femoral neck
Cysts in the femur are often an incidental finding and are diagnosed with a fracture using imaging. Cysts are benign masses that form in the cancellous bone of long bones. The cancellous bone is the inner part of a bone, which consists of so-called trabeculae and is therefore less stable than the outer layer (compacta).
Since a cyst in the thigh neck causes the bone to lose stability and the risk of a spontaneous bone fracture, the cyst is usually surgically removed. The resulting cavity is filled with a bone-like substance and the patient can continue to live without symptoms.