Inflammation of the parotid gland
Synonyms
Parotitis
General
The acute inflammation of the parotid gland (Technical term: parotitis) usually starts suddenly.
Many of the affected patients experience sudden discomfort and severe swelling in the cheek area while they are eating.

In most cases they are bacterial pathogens which penetrate through the duct into the parotid gland are responsible for the development of an acute inflammation of the parotid gland.
Both patients suffering from a chronic immunodeficiency suffer, as well as people with poorly adjusted Diabetes mellitus are particularly at risk of developing inflammation of the parotid gland.
In addition, especially during the pregnancy often observe flare-ups.
Another cause for the development of an acute inflammation of the parotid gland is a restricted supply of fluids and the associated throttling of the Saliva production.
Immigrated bacteria cannot literally be flushed out of the ducts of the gland due to a decrease in saliva secretion.
The risk of developing an acute inflammation of the parotid gland increases.
In addition to the bacterial pathogens, other factors can also be responsible for the occurrence of inflammatory processes in the area of the parotid gland.
In about 60 to 90 percent of the observed cases Salivary stones can be detected that impair the flow of saliva.
In most cases, however, it is not possible to precisely identify the cause. Rather, it is assumed that the acute inflammation of the parotid gland is a multifactorial disease acts in which the interaction of various risk factors makes a decisive contribution to the development of the disease.
This disease is a very common phenomenon. In some cases, the inflammation of the parotid gland is almost asymptomatic and is not perceived as a disease.
In general, it can be assumed that roughly every second to third person will experience at least one acute inflammation of the parotid gland in their lifetime.
Women are affected roughly as often as men. A connection between the patient's age and the likelihood of illness has not yet been proven.
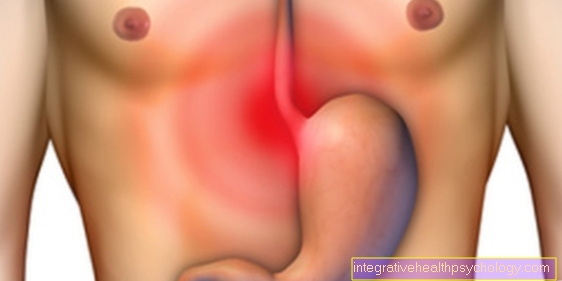
Figure inflammation of the parotid gland

Inflammation of the parotid gland
Parotitis
- Parotid gland -
Parotid gland - Parotid duct
(Execution of the
Parotid gland) -
Parotid duct - Upper jaw -
Maxilla - Temporomandibular joint -
Articulatio temporomandibularis - Salivary stone -
Sialolite - Lower jaw -
Mandible - Symptoms -
Swelling around the cheek,
Induration, redness, overheating,
purulent fluid in the mouth,
Fever, tenderness
Causes:
A - formation of salivary stones
(Saliva backlog),
bacterial infections, tumors,
poor oral hygiene,
weakened immune system,
Diabetes, medication (antibiotics)
Therapy:
B - stimulation of saliva production
(Chewing gum, lemon juice,
sour sugar-free candies)
C - massages of the
Parotid gland
D - Adequate hydration,
thorough and regular
Oral hygiene
E - taking pain relievers
Drugs (analgesics)
with ibuprofen or paracetamol
F - Operative removal
(large salivary stones),
Extracorporeal shock wave lithotripsy
(ESWL)
You can find an overview of all Dr-Gumpert images at: medical illustrations
Symptoms
The acute inflammation of the parotid gland manifests itself in most cases by the sudden appearance of the typical symptoms.
In many of the affected patients, the symptoms only manifest themselves on one side of the face.
Various triggers, however, provoke bilateral inflammation of the parotid gland and thus the bilateral appearance of the classic symptoms. If salivary stones are responsible for the development of the acute inflammation of the parotid gland, the symptoms can even occur some time before the actual inflammatory reaction begins.
However, this phenomenon is highly dependent on the size of the salivary stones. Regardless of the cause, the affected patients describe roughly the same symptom complexes.
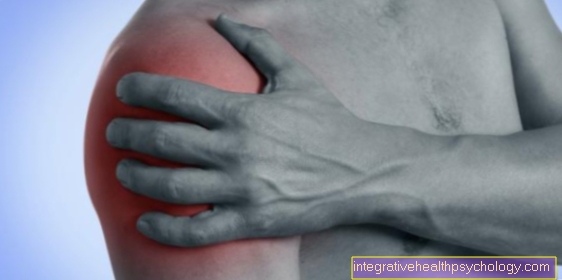
Pronounced swellings of the face or in the area of the cheek region can be observed, especially when eating.
In addition, most of those affected notice a significant hardening and tenderness on the inflamed half of the face.
The connection between "Increase in symptoms“And food intake can be explained quite simply. Inflammatory processes in the area of the parotid gland cause the tissue to swell and block the flow of saliva.
However, while eating, the parotid gland begins to produce larger amounts of saliva. This ultimately leads to a high pressure build-up within the gland. The affected patient feels pronounced pain, the swelling increases and the parotid gland hardens noticeably.
In addition to the local complaints, acute inflammation of the parotid gland in most cases also leads to the development of general symptoms.
Most patients develop a fever due to the inflammatory process. In rare cases, severe chills occur.
Furthermore, the skin in the area of the parotid gland is usually red and overheated. In very pronounced cases, purulent fluid is drained into the mouth during the course of the disease.
In these cases, patients notice an unpleasant taste.
The sometimes severe swelling can also block the jaw joint and make the chewing process more difficult. In most cases, the affected patients can hardly open their mouths.
The symptoms typical of an acute inflammation of the parotid gland can take on a very variable extent depending on the patient and the severity of the disease.
In some cases, the acute inflammation of the parotid gland is even completely without symptoms.
Only while eating does the blockage of the saliva flow trigger a slight swelling in the area of the cheek.
Also read: Symptoms of inflammation of the parotid gland and Swelling behind the ear
Inflammation of the parotid gland and toothache
Toothache often occurs together with inflammation of the parotid gland. Most of the time they are the reason for the inflammation the great salivary gland. A poor oral and dental care is known to lead to tooth decay and inflammation of the gums. If the mucous membrane on the molars is also affected, this can encourage an ascending infection.
The parotid duct is opposite the second molar towards the cheek and is a possible entry point for bacteria from the oral cavity. If the bacteria of the oral flora rise in the duct, they can infect the parotid gland.
In terms of time, toothache or inflammation of the oral mucosa usually occurs first before reactive inflammation of the parotid gland can occur. The decisive factor here is not how severe the toothache is, but only the spatial proximity of the affected tooth to the duct of the parotid gland. If severe toothache leads to reduced food intake, the production of saliva is additionally reduced so that the bacteria are not flushed out again when the saliva drains and the disease process is thus accelerated.
causes

Both infectious and non-infectious causes play a decisive role in the development of acute inflammation of the parotid gland.
The most common cause of acute inflammation of the parotid gland is the formation of salivary stones (Sialolite).
The deposition of a small saliva stone can block the duct of the parotid gland, causing saliva to back up. The oral cavity is naturally richly populated by bacterial pathogens.
These rise through the duct into the parotid gland. Without the presence of salivary stones, however, the bacterial pathogens can be flushed out with the flow of saliva. If, however, there is a pronounced blockage of the excretory duct, the bacterial pathogens multiply and set off an inflammatory cascade.
As a result, inflammatory processes develop in the area of the parotid gland. However, acute inflammation of the parotid gland is usually not triggered by a single factor. Rather, it is assumed that the acute inflammation of the parotid gland is a so-called "multifactorial disease“, In which the interaction of various risk factors makes a decisive contribution to the development of the disease.
You might also be interested in: Causes of a salivary stone
A change in the natural composition of the saliva can also be considered as a possible cause of acute inflammation of the parotid gland.
Especially the excess of calcium (Hypercalcemia) or a low liquid content should play a decisive role in this context.
In addition, patients with poorly controlled diabetes mellitus, gout and / or diseases that are associated with an impairment of the glandular ducts have a significantly increased risk of the disease. Especially in patients with cystic fibrosis (Cystic fibrosis), recurrent inflammation of the parotid gland can be observed. However, an increase in the risk of developing acute inflammation of the parotid gland can also have other causes.
Above all, anatomical constrictions, scar tissue or tumors can impede the outflow of saliva and thus promote inflammatory processes.
In addition, poor or inadequate oral hygiene can help increase the risk of developing acute inflammation of the parotid gland.
In addition to these known risk factors, a connection between the increased occurrence of inflammation of the parotid gland and disorders of the electrolyte and water balance has recently been assumed. D.
It can also be observed in everyday clinical practice that inflammatory processes in the area of the oral mucosa (Stomatitis) often have a tendency to extend into the parotid glands.
Overview of causes:
-
bacterial infections of the parotid gland
-
Parotid cancer
-
Obstructions to the outflow of the salivary gland ducts
-
Disturbances in the electrolyte and / or water balance
- Salivary stones
Medicines that reduce the flow of saliva:
- Diuretics
- Antidepressants
- Antihistamines
- beta blockers
- Viral diseases (e.g. mumps, cytomegaly, Coxsackie A virus)
- Autoimmune diseases (collagenoses, Sjogren's syndrome)
- Post-therapeutic (e.g. after radiation therapy)
Is inflammation of the parotid gland contagious?
Whether inflammation of the parotid gland is contagious depends on the cause of the inflammation.
Unilateral inflammation of the parotid gland is usually not contagious if adequate hygiene measures such as regular hand washing are observed. The bacterial pathogens can only have one Droplet infection or smear infection transmitted from the oral cavity. If the person concerned washes their hands after coughing or coming into contact with the oral mucosa, transmission of the pathogen is unlikely. Should a transmission nevertheless occur, bacteria that every person has in their own mouth are transmitted. The causative agents of a unilateral parotid gland inflammation are mostly Streptococciwhich are part of the natural oral flora in healthy people.
If there is bilateral inflammation of the parotid glands, it is a viral disease mumps obvious cause. In this inflammation of the parotid glands, which often occurs in childhood, the viral pathogens can about one day before the swelling occurs to about three days can then be transmitted to contact persons, making mumps contagious during this period.
The symptoms of the disease can be used as a rough guide for the contagiousness of parotid inflammation. If the person concerned has pain and swelling on one side, contact with others is not a problem. If the person also suffers from a fever and develops swelling in both parotid glands, they should stay at home and avoid unnecessary contact.
diagnosis
The diagnosis of acute inflammation of the parotid gland is usually divided into several steps.
In most cases, a detailed doctor-patient discussion (anamnese) guided.
During this conversation, the symptoms and the causal relationship of the complaints should be presented in as much detail as possible.
Both the quality and the exact localization of the symptoms perceived by the affected patient can provide a decisive indication of the underlying clinical picture.
The suspicion of the presence of an acute inflammation of the parotid gland usually arises from the information about at what time the symptoms first appeared and what factors caused them Increase in intensity.
The pain when chewing is typical of the acute inflammation of the parotid gland.
Following the doctor-patient conversation, a physical examination is typically carried out in which the affected body region (in this case the oral cavity and cheeks) must be carefully inspected.
In the case of acute inflammation of the parotid gland can typically be found in the area of the cheeks Hardening, swelling, redness and Overheating determine.
In many cases, external pressure causes purulent secretion emerges from the duct of the parotid gland. Ideally, this secretion should be collected and examined in a laboratory. That way the underlying Pathogen can be proven and targeted treatment initiated.
Furthermore, the oral cavity should be carefully inspected during the clinical examination as well as the Tooth status be collected.
A blood test is typically ordered afterwards. With the help of possible changes in the blood count (Increase in inflammatory factors; above all White blood cells and C-reactive protein) the presence of inflammatory processes can be proven.
In this context, however, it should be noted that an increase in the inflammation parameters is not necessarily indicative of the presence of inflammation of the parotid gland. The rise of white blood cells (Leukocytes) and C-reactive protein (short: CRP) can also be an indication of localized inflammation.
Searching for the cause also plays an important role in the diagnosis of acute inflammation of the parotid gland.
If it is suspected that a salivary stone could be responsible for the occurrence of the inflammatory processes, one should urgently Ultrasound examination (Sonography) be performed.
With the help of this examination method, the attending physician usually succeeds in detecting salivary stones from a size of approximately one and a half millimeters.
In addition, the ultrasound examination may serve this purpose Abscesses or Tumors to prove.
If the findings are unclear and / or the symptoms are particularly pronounced, additional imaging procedures may also be necessary.
In the diagnosis of acute inflammation of the parotid gland, the Magnetic resonance imaging (in short: MRI) and the Computed Tomography (CT) an important role.
In addition, in many cases the implementation of a Endoscopy of the parotid duct and a so-called "Fine needle puncture“Indicated for sampling.
The Sialography is an important diagnostic tool for acute inflammation of the parotid gland caused by salivary stones. This examination method shows both the glandular duct system and the gland itself. With help of a Contrast agent, which is administered to the patient via the vein, constrictions and / or blockages within the glandular duct system can be shown radiologically.
therapy

In the case of acute inflammation of the parotid gland, the choice of the appropriate method of treatment depends on various factors.
On the one hand, the fact whether the inflammatory processes were caused by a salivary stone plays an important role.
On the other hand, the choice of the best treatment method also depends on the severity of the clinical picture.
In general, if there is an acute inflammation of the parotid gland, the use of so-called "Saliva loosener“To stimulate saliva production.
In particular, the use of candies, chewing gum and drinks has so far proven itself in everyday clinical practice. Through a targeted Increase in saliva production and the increased secretion of thin secretions, the salivary gland and its ducts can be cleaned.
In many cases, the increased flow of saliva can even serve to flush small, canted saliva stones from the duct.
Since in the development of the acute inflammation of the parotid gland a direct or at least indirect bacterial involvement can be demonstrated in most cases, the Administration of antibiotics an important point in the treatment of affected patients.
In this context, however, it should be noted that acute viral inflammation of the parotid gland does not respond to antibiotic treatment and can usually only be treated symptomatically.
For the affected patient, the pain relief provided by ingestion pain reliever medicines (Analgesics) represents the most important treatment step.
Especially drugs that have the active ingredients Ibuprofen or Paracetamol have proven themselves in the treatment of acute inflammation of the parotid gland.
If an abscess has developed in the course of the inflammatory processes, in most cases one must surgical opening of the abscess cavity be performed.
The complete removal of the parotid gland is always necessary if inflammatory processes occur more frequently or a malignant tissue change is suspected (tumor) consists.
Salivary stones that cannot be flushed out by increasing secretion must be removed in another way.
In the case of salivary stones that are at the end of the excretory duct, the treatment can be carried out with the help of a Aisle slitting and regular Massages the parotid gland.
Salivary stones that cannot be felt from the outside and lie deep in the duct system can be removed with the help of the so-called "extracorporeal shock wave lithotripsy“ (in short: ESWL) are treated.
With this method, the salivary stone is relocated by sound waves from the outside. Large stones, however, usually have to be removed surgically.
homeopathy
If there is uncomplicated inflammation of the parotid gland, treatment with homeopathic remedies is possible. However, a doctor must ensure that there is no fever, no rotten tooth or an obstacle to the drainage of saliva from the gland. Only then can a safe treatment with homeopathic remedies be started.
Globules or drops off Ailanthus glandulosa (Tree of Gods) have proven to be effective and can work together with Schuessler salts how Potassium chloratum support healing. Also Belladonna globules (Belladonna) are said to have a healing effect.
In addition, drinking Sage tea stimulate the flow of saliva and thus “flush out” the pathogens from the inflamed parotid gland. sage It also has an anti-inflammatory effect. Basically, a homeopathic treatment should optimally balance the mineral balance of the person affected and stimulate the flow of saliva sufficiently so that the pathogens can be eliminated from the gland.
What home remedies are there?
If you want to treat an inflammation of the parotid gland with home remedies, anything that stimulates the flow of saliva is available. The increased flow of saliva flushes both the gland ducts themselves and the duct of the gland and thus transports the pathogens out of the inflamed tissue.
They are best suited for this Candy or chewing gum, whereby sour flavors stimulate saliva production particularly intensively. The saliva itself has the cleaning function already described, but with the help of its many enzymes also has an antibacterial effect.
If you want to further support the body's own healing, is one optimal oral hygiene a must. Brushing your teeth after eating and rinsing regularly will prevent bacteria from building up in your mouth and may remove pus that may have drained into your oral cavity.
If there is a purulent inflammation, should anti-inflammatory teas such as sage or chamomile tea (see also: chamomile) can be used. Drinking tea keeps the mucous membranes moist, disinfects them and keeps them elastic. This means that pathogens that remain in the mouth cannot damage the mucous membranes any further.
Those affected will quickly find out intuitively what helps them the most. It is important to drink enough fluids and continue to eat well and maintain your strength depending on your appetite. This is the only way the immune system is strong enough to fight the inflammation.
forecast
In most of the affected patients both shows the by one Salivary stone caused, as well as the acute infectious inflammation of the parotid gland, a favorable prognosis.
However, the prompt initiation of a suitable treatment method is a prerequisite for optimal healing. If the parotid gland has to be removed due to the inflammatory processes, this usually has no noticeable effect on saliva production. The remaining Salivary glands are mostly able to produce sufficient amounts of saliva.
How long does inflammation of the parotid gland last?
How long an inflammation of the parotid gland lasts depends on both what caused the inflammation and the treatment. Generally it takes time three to eight days until the inflammation subsides.
Care should always be taken to ensure that the cause is adequately treated, as treating the symptoms alone is ineffective in the case of inflammation of the parotid gland. The inflammation can only heal quickly if the saliva drains out of the parotid gland and good dental and oral hygiene is maintained.
The general and nutritional condition of the person affected also determines the healing process. In older people in particular, inflammation of the parotid gland can be more protracted than in children, who usually recover quickly. Of the The use of antibiotics only shortens the course of the disease if there is a bacterial inflammation by a couple of days. Any persistent inflammation of the parotid gland over a period of three to four days or with additional complications such as fever or pus evacuation in the mouth should be examined and treated by a doctor.
Prevention / prevention
Acute inflammation of the parotid gland cannot be prevented in every case. Nevertheless, the decisive risk factors can be reduced and the formation of salivary stones, the main cause of acute inflammation of the parotid gland, counteracted.
In this regard, great emphasis should be placed on thorough and regular Oral hygiene be placed. Patients who have already suffered from acute inflammation of the parotid gland should definitely ensure that they are drinking enough fluids.
Inflammation of the parotid gland during pregnancy
During pregnancy, the expectant mother's immune system is in a learning process. It has to learn to tolerate the embryo even though it has paternal characteristics that are alien to the mother. At the beginning of a pregnancy in particular, the immune system shuts down a little in order to protect the embryo from rejection. This guarantees complete nidation and training.
The downside is that the immune system is now at that time more susceptible to other pathogens is. This explains, for example, the occurrence of inflammation of the parotid gland. The parotid gland inflammation is a possible infection alongside others such as gastrointestinal infections and should be clarified by a doctor, but not be a major cause for concern.






.jpg)


.jpg)