Juvenile polyarthritis
definition

arthritis is a disease of the musculoskeletal system. Here it comes to a chronic inflammation one or more Joints. Juvenil means that Joint inflammation before the age of 15 must have occurred. Polyarthritis means that multiple joints must be involved.
In general, juvenile polyarthritis is counted among the autoimmune diseases. External factors are suspected to be the trigger of juvenile arthritis, e.g. viruses or bacteria as pathogens that can trigger the disease if there is an existing genetic predisposition. There are numerous locations in the DNA that can promote juvenile arthritis, but in most cases the gene areas are different from those in rheumatic diseases in adults.
Still's disease also belongs to juvenile polyarthritis and is therefore a sub-form. Read the following article to find out what distinguishes Still's disease from the other forms: Still's disease - what's behind it?
frequency
Every year around 5 to 6 in 100,000 children and adolescents under the age of 16 develop juvenile arthritis. As soon as several members of the family are affected, the risk of the disease increases tenfold.
An identical twin examination showed that there is an increased probability that the second child will fall ill about six months after the first.
Symptoms
The typical signs of joint inflammation with swelling, redness, overheating and pain are not as common in children as they are in adults. Many children do not express their pain right from the start, they tend to let their parents carry them around, are tearful and often tired.
A Relieving posture is taken in the affected joint, most often the joints are flexed. If this is not noticeable over a longer period of time, not moving the joint can make it permanent Shortening of muscles and tendons come. In the worst case it can lead to one asymmetrical outgrowth of the joints come.
By applying pressure to the affected joint, a moderate "Pressure pain" trigger. The children state that the pain usually gets worse in the morning or after a long period of inactivity. Likewise, a Morning stiffness to be watched.
The arthritis (Inflammation of the joints), which affects many joints, occurs first on the small joints of both hands and Feet on.
In the chronic form of juvenile rheumatoid arthritis with high disease activity, growth and development in relation to puberty may be impaired and weight loss may occur.
Juvenile polyarthritis, rheumatoid factor positive
The following criteria must be met: At least five or more joints must be in the first six months have juvenile joint inflammation. Must be in the blood Rheumatoid factor be detected. The test must be positive twice with an interval of three months.
The following diseases must be excluded:
- HLA-B27 positive arthritis in boys
- psoriasis of the child concerned or of a first-degree relative
- chronic inflammatory bowel disease such as Ulcerative colitis or Chron
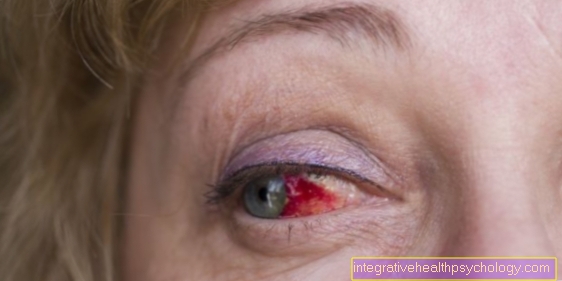
- Conjunctivitis of the eye (Uveitis)
- other known Rheumatic diseases like spondylitis, Sacroiliitis or enthesitis-related arthritis.
Juvenile polyarthritis with rheumatoid factor positive results occurs in 7 to 13 year olds, 90% in girls. Typical signs such as swelling, redness, pain, effusion can occur. It shows up Morning stiffness. This means that after sleeping or not moving for a long time, the joints are often stiff and painful. After moderate exercise, the pain will calm down and the joints will be easier to bend again.
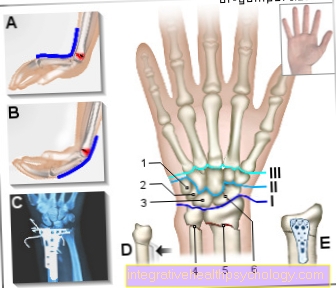
The inflammation occurs on both sides at the same time and occurs primarily in the wrist, finger, and toe joints, but basically any other joint can be affected as well. Kick frequently severe functional damage on that in part no longer
As with chronic polyarthritis in adulthood, it can also affect children and adolescents Rheumatoid nodules occur. Additionally, smaller and medium-sized Vessels and internal organs become affected by the inflammation.
Other symptoms of juvenile polyarthritis with rheumatoid factor positive are:
- Growth retardation up to a standstill
- delayed development
- Performance kink
- slightly increased temperature
- Weight loss
- Poor performance
- Swelling of the lymph nodes
- slight enlargement of the liver and spleen.
Serious consequences can occur quickly in the course of the disease. The disease activity can easily be read from the increase in the rheumatoid factor and the inflammatory activity, which can be measured using ESR and CRP in the blood.
Within a short time you can bony injuries occur, which can lead to limited mobility and joint misalignments. Therefore, an early diagnosis with immediate treatment is necessary and the progression of the disease can be stopped and a possible gradual cure can be achieved.
Juvenile polyarthritis, rheumatoid factor negative
The following factors must apply in order to develop joint inflammation in children and adolescents into juvenile polyarthritis without rheumatoid factor classify:
Five or more joints must become infected with inflammation in a six-month period.
In addition, the following must be excluded:
- psoriasis (psoriasis) in the child or first-degree relatives,
- HLA-B27 positive arthritis
- inflammatory bowel disease
- other rheumatic diseases
80% of girls between the ages of 2 and 16 are affected by this type of polyarthritis. At the start the disease show up often no pronounced symptoms. There is only a slight swelling with effusion and a slight overheating. Only the degrees of movement are usually noticeably restricted. Typical for the clinical picture is a symmetrical attack on the toes, fingers and wrists, but also cervical vertebrae and that Temporomandibular joint can be affected.
Diagnosis: In the blood count, a slight increase in the inflammation values (ESR, C-reactive protein) can be shown.
In the course of the disease of juvenile polyarthritis without rheumatoid factor it can become pronounced osteoporosis of the joints come. A irregular growth occurs because the inflamed joints often mature faster. In the course of time it usually comes to one Undergrowth with a regression of the muscles. Destruction of the joints is rare and only occurs later in the disease.
treatment
The goals of treatment are clearly defined. The aim is to alleviate the pain and bring the inflammation under control as far as possible. In addition, one tries to avoid joint damage and to achieve normal growth in the child. Uveitis, which can occur in both forms, is particularly dangerous. If left untreated, it can lead to visual impairment or even blindness.
Depending on the severity of the disease, the treatment is individually adapted to the child. Both physiotherapy and medication are used.
In physiotherapy, the restricted range of motion should be increased again through intensive training. Bad posture should be avoided or improved and the muscles trained. The treatment can be completed with cold or heat therapy as well as electrical treatment.
Studies show the positive effects of exercise. School sports can be done to a limited extent, jumping and running should be avoided. Physiotherapy alone is often not enough and drugs must be used.
Diclofenac, ibuprofen or indomethacin are often given at the beginning. They belong to the group of non-steroidal anti-inflammatory drugs and have anti-inflammatory and analgesic effects. They should be prescribed in about six to ten weeks. If there is no improvement at the end of this period, other drugs must be used.
These include glucocorticoids. They work very well, but they also have many side effects. Often these are injected into the joint and thus have a good local and less systemic (related to the whole body) effect.
If the symptoms of juvenile polyarthritis are severe, basic therapeutic agents (Disease modifying anti rheumatic drugs or DMARDs) into play. They can be prescribed in combination with the glucocorticoids and non-steroidal anti-inflammatory drugs.
However, it takes two to three months for the effects to occur. Methotrexate, sulfasalazine, or azathioprine are often given for up to nine months to effectively contain the disease.
So-called biologics, which are also called DCARDs "Disease Controlling Anti Rheumatic DrugsThese include Etanercet, Tocilizumab, Infliximab, Adalimumab, Anakinra and Rituximab, all of which intervene differently in the inflammation chain and block it. They work very well and can treat severe forms of juvenile polyarthritis that are not contained on methotrexate or other DMARDs could be prescribed.