Adult rubella
definition
Rubella is caused by the rubella virus, which belongs to the togavirus family. Rubella is a teething problem. The typical age peak is between 5 and 9 years of age, but adults can also be affected. In recent years there has been an increasing number of infections in young adults.
See also: Symptoms of rubella
The infection is particularly dangerous during pregnancy. Pregnant women are therefore particularly at risk if there are gaps in vaccination coverage. After a rubella infection, there is lifelong immunity. If the rubella breaks out, notification is mandatory.
Also read: Vaccination during pregnancy
causes
An infection with rubella happens via a so-called Droplet infection from human to human. The pathogens are transmitted to another person in saliva or nasal secretions when coughing and sneezing. Man is the only known host. The rubella virus is absorbed via the respiratory tract and initially multiplies in lymph node stations and then spreads further in the blood.
There is a risk of infection about one week before to one week after the rash appears. However, the actual risk of infection is generally classified as not very high. A special form of infection occurs during pregnancy. If the mother is infected with rubella, she can transmit the virus to the unborn child through the blood of the placenta. The sick children can be contagious for up to a year after birth.
Please also read: Rubella During Pregnancy
Symptoms
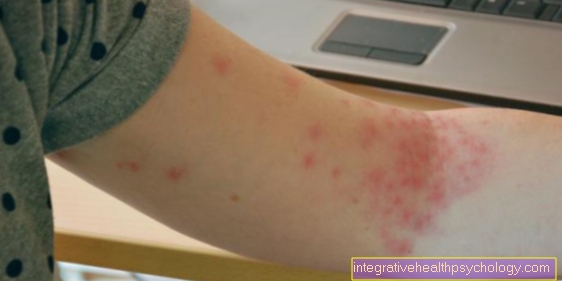
Before the typical Rash the affected person feels weak and shows signs of a mild cold. The typical rubella rash (exanthema) begins on the head, usually behind the ears, and from there it spreads over the whole body including the extremities. It is composed of fine to medium-spotted red dots. These are light red and are usually easy to distinguish from one another. The rash is described as fleeting, as it usually disappears after a few days.
Also read: Causes of rash with red spots.
Those affected, mostly children, are often only slightly affected. The feeling of illness with headaches and body aches is only slightly pronounced. There is often a subfebrile temperature increase of up to 38 ° C. In rare cases, a high fever actually occurs. As an immune reaction to rubella infection, the lymph nodes swell as defense stations of the body, characteristically in the neck and behind the ears (see also: Causes of swelling of the lymph nodes behind the ear). Sometimes an enlarged spleen can also be felt (see also: Spleen pain). As an accompanying reaction, slight cold symptoms, especially runny nose, can occur. Also one Conjunctivitis of the eyes is possible. The blood count shows an unspecific drop in white blood cells (leukocytopenia).
course
In the vast majority of cases, the course of a rubella infection is harmless and very mild. In half of the cases, the outbreak does not even occur. Complications mainly occur in adulthood. They range from Joint pain up to very painful inflammation of the joints (arthritis). These can persist weeks after the rash has subsided. The general inflammatory reaction can also spread to a large number of organs.
Also read: Rash and joint pain
It happens regularly to Otitis media or one bronchitis. Inflammation of the brain is particularly dangerous Encephalitis or an inflammation of the heart muscle or the pericardium in the form of a Myocarditis or. Pericarditis. In the aftermath of the infection, there may be a drop in blood platelets (thrombocytopenia), which in turn provokes the slightest bleeding into the skin.
The course of the disease is particularly dramatic during pregnancy. An abortion or a premature birth can be the consequences. The extent of the complications varies depending on the time of illness. In the first ten to twelve weeks of pregnancy in particular, there is a 50% chance of transmission from mother to child and thus of rubella embryopathy. This so-called Gregg triad consists of Heart defects, clouding of the lens (Cataract) and Inner ear hearing loss. A limitation of the cognitive abilities (mental retardation) is also possible. After the first trimester, rubella fetopathy can lead to changes in the blood count, inflammation of the liver (hepatitis) or an enlarged spleen (splenomegaly).
How contagious is rubella to adults?
Since most adults have adequate vaccination protection, rubella is no longer a major threat. However, it is just as contagious as it is for children. Rubella is a typical childhood disease, but it can also affect adults. If the vaccination protection does not exist or is unclear, it should be checked urgently and taken up. This is generally recommended for all adults, but especially for women of childbearing age. In pregnant women, determining the titer of the immune body IgG against rubella is therefore a standard precaution. If the titer is over 1:32, it can be assumed that the pregnant woman and her unborn child are adequately protected.
Which adult needs a vaccination?
According to the recommendation of the STIKO vaccination commission, the rubella vaccination in combination with the measles and mumps vaccine (MMR vaccine) should be carried out between the ages of 12 and 15 months. A repetition should take place before the age of 2 to avoid possible vaccination failure in so-called non-responders. It is a live vaccination. This means that weakened pathogens are injected, which are supposed to encourage the body's own immune system to develop antibodies against the actual pathogen.
If the vaccination was missed in childhood, vaccination should also be given in adulthood. This is also the case if the person concerned has already gone through rubella. After an infection, there is basically lifelong protection. However, if this rubella disease was a long time ago, a new infection can occur in rare cases. A catch-up vaccination is therefore also recommended in adulthood. Vaccination is particularly important for women who are of childbearing age, as infection of the unborn child is particularly dangerous.
The vaccination may cause redness, swelling or hypersensitivity at the injection site. Fever is also possible. Since it is a live vaccination, it can potentially lead to a milder course of rubella.
Also read our main article on the topic vaccination
Read more on the topic: MMR vaccination
How long is the incubation period?
The incubation period means the time between infection and the appearance of the first symptoms. For rubella it is approx two to three weeks. In half of the cases, the disease does not break out at all and is asymptomatic.
Duration
The rash only lasts for a few, usually 3, days. The feeling of illness usually begins a week beforehand and can continue for a few weeks afterwards. Especially in adults there is an increasing progression with complications such as joint pain.
diagnosis
A differentiation from other childhood diseases with rash such as measles, Ringlet rubella or Scarlet fever is often not that easy. The diagnosis is usually made clinically and only requires further diagnostic steps in special cases. Direct detection of the pathogen, for example from the throat secretion, is not part of the standard procedure, as it would not have any therapeutic consequences.
On the other hand, if you want to be on the safe side with pregnant women or newborns, antibodies are determined in the blood. Since this result can often appear false positive, there is also the hemagglutination test, in which red blood cells clump together, to confirm this. Further detection possibilities are possible via cultural cultivation, via a PCR (here the genetic material of the virus is detected) of the amniotic fluid or a sampling from the placenta villi.
treatment
Since rubella is a virus, like most viral diseases, one comes in symptomatic treatment into consideration. As opposed to a bacterial infection, attack Antibiotics not here. Symptomatic therapy is based on antipyretic agents z for example with Ibuprofen or Paracetamol. At the same time, these alleviate pain in the limbs or headaches. Adequate hydration is also important.
If pregnant women had contact with rubella infected people is one passive immunization with immunoglobulins possible within three days of initial contact. However, this does not prevent infection 100%. If the infection occurred during pregnancy, the complications of rubella embryo fetopathy must be treated. In addition to intensive care, the children may need operations on the heart or the eyes after birth, as the rubella virus can lead to malformations of these organs in the unborn child.



.jpg)