Fistula in the genital area - everything you should know
introduction
Fistulas are a common problem that is not unique to the genital area.
A fistula usually describes a tubular connection between two hollow organs in the body.
The two hollow organs are physiologically separated from each other and the two anatomical regions can only be connected to one another through a chain of certain causes. The symptoms are accordingly very different and can be harmless to serious.
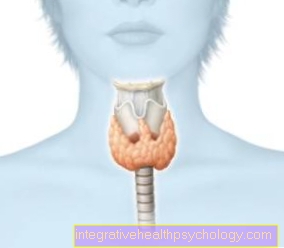
In women, the cavities of the genital area mainly include the vagina but also the uterus.
In men, fistulas with organs of the genital tract are very rare and unusual.
In women, the vaginal canal is particularly affected by fistulae, which in most cases forms fistulas with parts of the intestine or parts of the urinary system.
In most cases, fistulas in the genital area do not represent a medical emergency, in contrast to arteriovenous fistulas, which can sometimes be life-threatening.
However, the effects of such a fistula can be very unpleasant for the women concerned, which is why treatment is indicated in any case.
The healing possibilities are very good, especially through surgical interventions.
For more information on how to treat fistulas in the intestine or the anus, see: Fistula in the intestine and fistula in the anus

These are the causes of a fistula in the genital area
The causes of a fistula formation can be numerous.
However, they all have in common that there is a change in the intact vaginal wall, which can damage the wall structure in several levels.
With close spatial proximity to the bladder, urinary tract or intestinal loops, the walls of the organs can grow together in the following regeneration phase and form small tubular connections.
This manipulation is often caused by inflammation of the genital, urinary tract or intestine.
In the genital area, these can mainly be fungal diseases, sexually transmitted diseases and other infections caused by pathogens.
In the intestinal area, fistula formation can also be traced back to pathogens, for example in the context of diverticulitis with inflamed protrusions of the large intestine.
Chronic inflammatory bowel diseases are also an important cause of fistula formation, especially Crohn's disease and ulcerative colitis.
Malignant tumors are another important cause of fistula formation.
For example, bladder cancer, cervical cancer or rectal cancer can cause fistulas through their invasive growth through the organ walls.
Very rarely, malformations of this type can be congenital in women.
Both the fistula of the vagina to the intestine and the fistula to the bladder can occur as embryonic malformations.
Apart from diseases of the organs, all accidents and injuries are also risk factors for fistula formation.
Injuries to the intestinal or genital walls can occur, for example, during operations, childbirth, vaginal examinations or through autoerotic accidents.
If you would like more information about the tumor diseases listed above, please also read our articles: Urinary bladder cancer and cervical cancer
What is the prognosis for a fistula in the genital area?
The general prognosis for the treatment of fistulas is good.
The success of treatment and the duration of the disease vary primarily with the size of the fistula.
Large defects, especially in the intestine, can require weeks of treatment and healing cannot be guaranteed.
In particular, concomitant diseases such as Crohn's disease, but also underlying causative cancer diseases, play an important role.
In general, over 90% of fistulas can be cured in the first attempt at treatment.
If the fistula recurs, however, the prognosis is worse, since the defective tissue increasingly loses the ability to heal due to previous operations
Do you have Crohn's disease and want to know how to treat it? Then find out more about it in our article: Therapy of Crohn's Disease
How is a fistula in the genital area treated?
The treatment of the fistula depends on the size of the defect, but in most cases it must be done surgically.
Here, too, the distinction between the fistula to the urinary bladder and the fistula to the intestine is crucial.
A urinary fistula to the vagina can often heal on its own.
It is advisable to drain the urine with the help of a urinary catheter to aid healing.
This allows the fistula to heal without coming into contact with urine.
Otherwise this could prevent the tissue from an optimal healing process.
Even after the fistula has closed, the urine should continue to be drained for a few days in order to protect the tissue for the time being until it has stabilized.
Even with a fistula from the intestine to the vagina, it may be necessary that the stool be drained away from the fistula until the time of healing.
Since this is associated with a major intervention and the creation of an artificial bowel outlet, this method is only used for large defects.
The large fistula can be treated surgically a few weeks after the anus has been created.
The tissue then has to heal well, which is not always guaranteed with certain previous illnesses.
The anus can be moved back after the surgery.
However, if cancer or inflammatory bowel disease is the cause of the fistula formation, treatment of the underlying disease is an important part of therapy.
Can a fistula in the intestine also heal on its own?
Smaller fistulas in the intestine heal on their own.
Many enterovaginal fistulas arise from inflammation of the genital tract or the intestine and can also heal again after the inflammation has been overcome.
In many cases there are smaller asymptomatic fistulas that go unnoticed and close by themselves.
Even symptomatic, smaller fistulas can heal on their own if the condition is good and the conditions are suitable.
Many of the defects can also be repaired in minor surgical interventions.
Only in the case of very large fistulas with severe symptoms should an artificial anus be considered and a lengthy course with surgical treatments.
You can read about the prognosis and the correct therapy for a fistula on the navel in our article: Fistula on the navel - you should know that!
These symptoms are accompanied by fistula
Symptoms of a fistula in the intestine
Fistulas between the vagina and parts of the intestine can appear due to changes on either side of the fistula formation.
The size of the fistula is decisive for the symptoms, the treatment method and the prognosis.
The symptoms of a large so-called "enterovaginal" fistula can be extremely uncomfortable and stressful for those affected.
Stool can enter the vagina through the fistula, which can lead to fecal incontinence, vaginal stool, foul-smelling discharge, and vaginal flatulence.
There is also potential inflammation caused by the stool in the genital area.
It is not uncommon for this to result in further pain, burning or itching and severe shame, as well as a restricted sex life.
Has your doctor diagnosed you with a fistula in the bowel? Then find out more about it in our article: Fistula in the intestine - causes & therapy
Symptoms of a fistula in the bladder
The fistula in the bladder is associated with fundamentally different symptoms than the fistula in the intestine.
In this case one speaks of so-called "urogenital" fistulas.
The main problem with this condition is urinary incontinence.
The urine can pass directly from the bladder or the area of the fistula into the vagina and flow out, since the vagina does not have a suitable sphincter muscle for urinary continence. On the other hand, when vaginal secretions enter the bladder, infections of the urinary tract can occur.
Abdominal pain, burning sensation when urinating and bleeding are typical. Sometimes the infection can rise to the renal pelvis, which often leads to a strong feeling of illness, fever and pain in the back.
The formation of fistulas in the bladder is less common than in the intestine.
In the case of newborns, a congenital malformation of the urogenital tract must be considered.
Diagnosis of a fistula in the genital area
At the beginning of the diagnosis, the patient is precisely questioned and examined.
Symptoms such as urinary incontinence or unusual vaginal discharge can be important indicators of a fistula.
In some cases, the opening and fistulae of the vaginal wall can already be recognized during the first vaginal examination.
In any case, the physical examination must be followed by apparatus-based diagnostics in order to be able to determine the exact course, extent and possibly the cause of the fistula.
This is understood to mean a diagnosis using electronic medical devices.
First, an ultrasound scan can be performed to suspect the course and size of the fistula.
Depending on the exact location of the fistula and the involvement of other organs, bladder or colonoscopy may follow, as well as X-ray and MRI examinations, also with contrast media or in the form of a so-called "urogram", in which the urine flow can be examined radiologically.