Swollen joints
definition
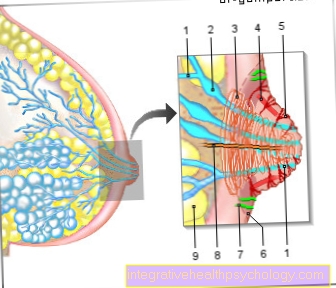
With a swollen joint, various structures in the area of the joint can be swollen, such as ligaments, tendons or capsules. A swollen joint is often caused by fluid accumulation in the joint cavity, known as joint effusion. Most of the time, an effusion occurs as part of an injury or inflammation. The accumulated fluid can also be purulent (infectious cause) or bloody (mostly traumatic cause) depending on the cause.
causes
There are various possible causes for a swollen joint. On the one hand, it can be an overuse of the joint, which often occurs in the knee joint. Even acute injuries such as a meniscus tear or cruciate ligament tear usually lead to joint swelling and associated joint effusion. Joint swelling can also occur in the case of osteoarthritis that occurs frequently with increasing age, which is wear and tear on the joints due to cartilage wear. In addition to these clinical pictures, bacterial or viral inflammation can also trigger joint swelling, this is known as arthritis. Bacterial inflammation can occur, for example, in the context of syphilis, tuberculosis or borreliosis, as well as being the result of a gastrointestinal infection or a urinary tract infection - typical pathogens for this are chlamydia and salmonella, which is referred to as reactive arthritis. Systemic diseases such as psoriasis or inflammatory bowel diseases such as Crohn's disease and ulcerative colitis can also be accompanied by joint swelling.
If several joints are swollen at the same time, this first makes the doctor think of a rheumatic disease. The rheumatic diseases include many different clinical pictures. What they have in common is that the body produces antibodies that are directed against the body's own structures and thus trigger inflammation that damages the joints. Typical symptoms are morning stiffness, improvement of pain / mobility throughout the day, pain (in contrast to osteoarthritis), which is also present at rest and is most pronounced in the morning.
Menopause
During the menopause, women are often affected by joint problems. The symptoms often move from one joint to the next, so women affected often fear that they are suffering from rheumatism. The hormone progesterone is responsible for joint problems during menopause, which is particularly effective during pregnancy and is responsible for maintaining pregnancy. Another effect of progesterone is to loosen the connective tissue. During the menopause, the level of progesterone and estrogen drops drastically and opposing effects become noticeable: In the case of the joints, the joint membranes harden. These hardenings are usually accompanied by pain at the beginning and sometimes also lead to poor mobility of the joint. These joint problems during menopause are sometimes accompanied by swelling of the affected joint. Of course, not all joint complaints / joint swelling in the menopause have to be traced back to the menopause itself, typical causes can still come into question.
You might also be interested in this topic: Menopause symptoms
Appointment with ?

I would be happy to advise you!
Who am I?
My name is dr. Nicolas Gumpert. I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
In order to be able to treat successfully in orthopedics, a thorough examination, diagnosis and a medical history are required.
In our very economic world in particular, there is too little time to thoroughly grasp the complex diseases of orthopedics and thus initiate targeted treatment.
I don't want to join the ranks of "quick knife pullers".
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You will find me:
- Lumedis - orthopedic surgeons
Kaiserstrasse 14
60311 Frankfurt am Main
You can make an appointment here.
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
For more information about myself, see Lumedis - Orthopedists.
Concomitant symptoms
The swollen joint is usually accompanied by movement-dependent pain and restricted mobility. Often there is also pressure sensitivity in the area around the joint. If inflammation is the trigger, one can often observe the five cardinal signs of inflammation: swelling, overheating, redness, pain and impaired function. If fever accompanies joint swelling, it is relatively safe to assume a bacterial or viral inflammation as the cause of the swelling, in which case a doctor should be consulted for therapy. If a bluish discoloration develops accompanying the swelling of the joint, this should also be clarified by a doctor, as it is probably due to bleeding in the joint.
Morning stiffness is typical accompanying complaints in rheumatic diseases and osteoarthritis. The patient needs about 30 minutes until he can move the affected joint properly again and the pain improves. As a result, mobility improves during the day through exercise. Osteoarthritis is also called initial pain, where the pain occurs at the beginning of a movement and improves over the course of the movement. For example, pain initially occurs when walking after long periods of sitting or standing.
Also read our topics: Rheumatoid arthritis and symptoms of osteoarthritis
Swollen joints with red spots
If red spots accompany one or more swollen joints, this may or may not be related to one another. The cause of the appearance of the red spots in combination with joint swelling can for example be psoriasis (psoriasis), which in some patients also occurs with joint involvement. The rash is usually stretched and, as the name of the disease suggests, scaly.
Lupus erythematosus, a rheumatic inflammatory disease, can also be associated with joint problems and a skin rash (especially in sun-exposed areas). In addition, there are other symptoms, such as the characteristic butterfly-shaped reddening of the face. The disease occurs mainly in young women. Also with Lyme disease, joint problems in an advanced stage can be accompanied by a red spot. This red spot is the tick bite, as a carrier of Lyme disease, a red rash spreads out and about, which is why it is also referred to as wandering redness. Rheumatic fever, which typically occurs in children, is one of the main symptoms associated with joint discomfort / joint swelling. The so-called Erythema nodosum, a red very painful lump, as well as that Erythema annulare, a ring-shaped reddening mostly on the trunk.
Swollen joints with pain
Pain is a typical symptom accompanying a swollen joint. Pain is actually always present, especially with traumatic joint swelling. In the case of inflammatory events, pain is also a typical symptom complex. With rheumatic complaints, pain also occurs both at rest and under stress. A joint swelling occurs in very few cases without pain.
Swollen joints with fever
If joint swelling is accompanied by fever, the first suspicion is that it is an infectious joint effusion, i.e. a bacterial or viral joint inflammation. The pathogens can, for example, have migrated into the joint through an inflammation of the gastrointestinal tract or urinary tract, which is usually referred to as reactive arthritis. Such joint inflammations often develop after an operation on the joint, for example as part of a joint puncture. With such interventions, of course, the attempt is always made to work as sterile as possible, but unfortunately one can never completely rule out inflammation as a complication.
If joint problems occur in children between the ages of five and fifteen, about two to three weeks after a respiratory infection, one should also think of rheumatic fever as the cause. Streptococci are the cause of rheumatic fever. Antibodies that are formed by the body against streptococci not only attack the bacteria, but unfortunately, in the case of rheumatic fever, also the body's own structures. However, rheumatic fever now only occurs very rarely due to the targeted administration of penicillin.
diagnosis
Joint swelling can usually be diagnosed by simply looking at it and feeling the joint. However, it is more difficult to identify the cause of the swollen joint. It is important for the doctor to know since when the joint swelling has existed, whether it was related to a trauma / injury, whether only one joint is affected, and whether additional symptoms such as fever have occurred. It is often possible to differentiate between a traumatic and an inflammatory cause. The doctor then examines the joint in detail, paying particular attention to typical signs of inflammation, such as reddening and overheating. In some cases, this is followed by an ultrasound examination, with which, above all, the extent of a joint effusion can be assessed. If an inflammatory or rheumatic origin is suspected, a blood test and a joint puncture usually follow. If the doctor suspects joint wear as the cause, an X-ray examination is a good choice for diagnosis. If joint injuries, such as those typical of the knee, are suspected (e.g. meniscus tear, cruciate ligament tear), the best way to assess the suspected cause is with magnetic resonance imaging (MRI).
Treatment / therapy
Often no treatment is necessary for a swollen joint and the swelling disappears on its own after a few days. It is especially important to take care of the affected joint; this applies above all to joint swelling that has come about as a result of overloading or injury. Cooling applications are often used as a support. Cold packs wrapped in towels (not without an envelope, otherwise you could freeze) or cooling ointments can be used for this. The application of heat is rarely useful and sometimes even counterproductive.
In the case of osteoarthritis, heat applications can provide partial relief. In addition to cold applications, analgesic and anti-inflammatory preparations can be used. These preparations are mostly used in the form of locally applicable gels. For example, Voltaren® with the active ingredient diclofenac is popular. Medicines such as diclofenac, ibuprofen or acetylsalicylic acid can also be used in tablet form. If there is an inflammatory cause of the joint swelling, the doctor can inject cortisone and sometimes a light anesthetic into the joint space for relief. If there is a strong accumulation of fluid, which is associated with severe restrictions for the patient, the doctor will perform a joint puncture to remove fluid and thus relieve the joint. The puncture does not help to remove the cause of the swelling, but only acts as a symptomatic, discomfort-relieving procedure. In addition, the puncture has the benefit that the removed fluid can be examined for pathogens or other abnormalities and thus, if necessary, the cause can be inferred. In the case of osteoarthritis, joint-gentle sports are generally recommended, including swimming and cycling.
Also read our topics: Therapy of osteoarthritis and therapy of rheumatoid arthritis
Duration
How long a joint has been swollen cannot be answered across the board, it depends on the underlying cause. If it is a sports injury, the swelling usually subsides after a few days. If there is an underlying rheumatic disease, the swelling can persist for weeks. Symptoms persist longer, especially with rheumatic diseases. If the swelling of the joints persists for six weeks or longer, a rheumatic disease becomes more likely.
Swollen joints especially on the hands / fingers
When it comes to joint swelling in the fingers or hands, one often thinks of rheumatic diseases such as rheumatoid arthritis. Joint swelling due to a joint injury occurs less often in the hand / fingers than in the knee or ankle, for example. Unfortunately, rheumatic diseases often first manifest themselves in the finger joints. Usually several joints are affected. It is typical of rheumatic diseases that these are accompanied by morning stiffness of the affected joints. Especially if the symptoms persist for more than six weeks, you should look specifically for a rheumatic disease. In addition to rheumatic diseases, osteoarthritis symptoms on the fingers are not uncommon. How can you differentiate between osteoarthritis swelling and rheumatoid swelling? An important clue for this is the location of the swelling. Arthrosis often affects the articular joints of the fingers, which are typically never affected in rheumatoid arthritis. The thumb saddle joint is also frequently affected by osteoarthritis and therefore more indicative of osteoarthritis. The middle joints are also often affected, while rheumatism usually affects the basic joints.
You might also be interested in this topic: Swollen fingers and hands
Swollen joints after exercise
If joint swelling occurs after exercise, this can indicate overload. A typical joint for an overload is the knee joint, for example after jogging or playing football. The affected joint should be spared for a few days after overloading, as this usually causes the swelling to recede on its own. However, if the swelling persists, a doctor should be consulted for clarification. Joint swelling after exercise can also be related to an injury, more common in team sports such as soccer. The event that ultimately led to the swelling does not have to have been so drastic that it immediately leads to the termination of the sport, but can also have been caused by a collision in which the swelling only develops slowly after the sport has ended. In the case of joint swelling after exercise, it is important to protect the joint for a few days and, if possible, to cool it.
You might also be interested in the following theme: The most common sports injuries