Oral lichen planus
What is oral lichen planus?
Oral lichen planus is also called lichen planus because it affects the mucous membranes (mucous membrane = mucosa). It is one of the most common accidental skin diseases in the world. It mostly occurs in people between the ages of 30 and 60. In addition to the oral mucosa, the tongue and lips are also affected. The mucous membranes of the genitals and anus also show abnormalities.
Oral lichen planus is a special form of conventional lichen planus. This means that the usual areas of skin are also affected: wrists, hollows of the knees, lower legs and lower back. A rare variant of the oral lichen planus is the so-called lichen planus erosivus mucosae. It is characterized by a particular painfulness.

The reasons
So far, no precise cause for the development of oral lichen planus has been found, which is why it is of idiopathic origin (coincidence). Viral infections with hepatitis B or C are now suspected as risk factors for normal lichen planus. Dental metals (metal substances in dental treatment) and spices may also play a role. When it comes to dental metals, mercury, chromium, cobalt, nickel, amalgan and gold are suspected. Thermal stimuli are also discussed.
Find out all about the topic here: Lichen planus.
The symptoms
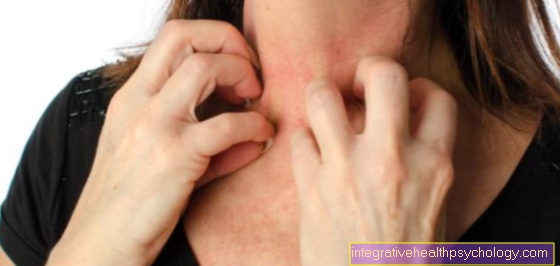
Oral lichen planus usually manifests itself with pain in the affected areas of the mucous membrane. With the special form of lichen planus erosivus mucosae, these can be almost unbearably painful. The general symptoms of lichen planus are usually also present. Sometimes those affected also complain of severe itching on other areas of the skin. These phases of itching occur in bursts.
In the course of this, the tongue may shrink (atrophy) with loss of the taste buds and thus the ability to taste.
Read more about the topic here: Lichen planus.
The diagnosis
First and foremost, it is a visual diagnosis by an experienced dermatologist. He combines the affected parts of the body with the typical appearance of the changes in the mucous membrane. These are called Wickham strips. It is a whitish, net-shaped arborizing drawing in the form of a branch growth near a tree crown ("arborizing"). There are no papules on the cheek mucosa or tongue (important in differentiating from other diseases).
In the process, the tongue shrinks (atrophy) with loss of the taste papillae. and painful erosions. The examiner must distinguish whether it is also a contact allergy to prosthesis materials and ask whether a specific sexually transmitted disease exists (secondary syphilis). If the picture is unclear, an examination of the cells can be ordered, as the so-called heat shock proteins HSP-60 are suspected of being involved in the disease process.
The treatment
The normal lichen planus usually disappears on its own after one to two years without therapy. Oral lichen planus, on the other hand, can persist longer. Local treatment methods are used for mild forms of the disease and mild symptoms. These can be creams with glucocorticoids, retinoids (vitamin A derivative) and ciclosporines. In severe cases, all of these agents can also be given systemically, i.e. as a tablet or infusion. Antihistamines help against itching.
In addition, the most important pillar of therapy is light therapy, called PUVA. The respective (slime) skin areas are irradiated with UV-A light. Before that, the skin was made sensitive, i.e. particularly receptive, to light with a substance called psoralen. In general, abstinence from nicotine and alcohol has a positive effect on the mucous membrane and promotes wound healing.
Prognosis
Long-term ulcerative changes are regarded as a precancerous stage (precancerosis). As a cancer, the spinocellular carcinoma can develop in 5% of cases as a result of the chronic inflammatory stimulus. Therefore, patients with oral lichen planus should be inspected by a doctor every 3 months. If necessary, he can also order biopsies, i.e. taking tissue samples.
The spontaneous healing rate is less than 5%. Therefore, proper therapy should always take place.