Causes of Thrombocytopenia
introduction
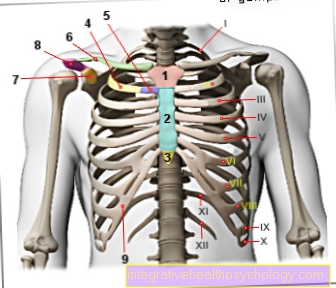
Thrombocytopenia describes a clinical picture in which the number of thrombocytes (blood platelets) in the blood is reduced. The causes can be broadly divided into two categories. Either there is a disorder in the bone marrow, so that the formation of platelets is reduced, or there is an increased breakdown, which is associated with a shortened life span of the platelets. The platelets play an important role in blood clotting. It follows that the first symptom of a deficiency is small, spontaneous bleeding into the skin and mucous membrane.
Read more on the topic: Thrombocytopenia

What are the possible causes of thrombocytopenia?
Educational disorders:
-
Fanconi anemia
-
Toxic from drugs, radiation or chemicals
-
Infections
-
Cancer - especially acute white blood cancer (acute leukemia), lymph gland cancer and bone metastases
-
Osteomyelosclerosis
-
Folic acid or vitamin B12 deficiency
Shortened service life:
-
Antibodies to platelets due to
-
Idiopathic Immune Thrombocytopenic Purpura (ITP)
-
Tumors, autoimmune diseases, HELLP syndrome
-
Medicines, blood products
-
-
Increased consumption due to
-
mechanical damage
-
Hemolytic uremic syndrome
-
increased coagulation activity
-
Enlargement of the spleen
-
Find out all about the topic here: The decreased platelet count.
Congenital educational disorders
The only congenital disorder of platelet production is Fanconi anemia. It is inherited as an autosomal recessive trait and weakens the entire bone marrow. This means that not only are the platelets depleted, but also all the other blood cells made by the bone marrow. It is a rare disease that continues to be associated with changes in the skeleton and organs. Often the patients are rather small and have a small head circumference.
About half of all patients with Fanconi anemia will develop malignant diseases of the blood system such as white blood cancer (leukemia) at some point in their life. Children with Fanconi anemia show symptoms such as fatigue, bleeding on the skin or mucous membranes and frequent infections early on. These symptoms can be explained by the damage to the bone marrow. It follows that particularly severe infections and cerebral hemorrhages are very much feared in these patients. The therapy consists of checking the blood count at close intervals and, if necessary, replacing the missing blood components with blood products.
This article might also interest you: Anemia
Acquired educational disabilities
There are a variety of acquired platelet formation disorders. Most are based on damage to the bone marrow, which limits the production of platelets. Medicines such as chemotherapeutic agents can cause this damage, which has to be accepted in order to be able to fight the tumor cells accordingly.
Radiation, which is also important in tumor treatment, can also damage the bone marrow. Cancer itself, as well as other malignant diseases of the bone marrow, such as osteomyelosclerosis, can lead to educational disorders. Certain chemicals such as benzene, which is used in solvents, also belong to this group.
In addition to the toxic causes, infections such as the HI virus also play a role. The virus mainly attacks immune cells, which contain a certain characteristic on their surface. This results in the dreaded immunodeficiency in these patients. In addition, the patients also develop thrombocytopenia.
Autoimmune diseases, i.e. diseases in which the body's own structures are attacked by the immune system, also belong to the acquired educational disorders. In this group of diseases, the progenitor cells of the platelets are fought by the immune system so that they can no longer develop into platelets.
Shortened lifespan: antibody reactions
An antibody reaction against the platelets without any other underlying disease is described by the clinical picture Idiopathic Immune Thrombocytopenic Purpura (ITP). In this disease, the body produces special proteins (antibodies) against the platelets, which are recognized and broken down by the immune system. As a result, the degree of thrombocytopenia varies. It has not yet been sufficiently clarified how this misdirected reaction of the body occurs. It is believed to be caused by mundane viral respiratory infections.
It is important to note that ITP is the most common cause of bleeding tendencies in children. How strong this bleeding tendency is depends on the number of platelets still present. There may be patients who show no symptoms at all, right up to patients who are covered with small hemorrhages (petechiae) all over their bodies. Enlargement of the spleen is rather untypical. A blood test is performed to diagnose ITP. An isolated reduction in platelets without the other blood cells showing abnormalities is typical. Many platelet precursor cells are found in the bone marrow, as the body notices the platelet deficiency and the bone marrow stimulates increased production.
In addition, the antibodies against the platelets can be detected using special methods. It is important that the ITP is a diagnosis of exclusion. This means that all other possibilities for this thrombocytopenia must first be ruled out before the diagnosis can be made. Therapy depends on the severity of the thrombocytopenia. Patients without symptoms can be monitored without further therapy. Symptomatic patients are initially treated with high-dose glucocorticoids. If this does not lead to success, the administration of immunosuppressants or immunoglobulins can be considered. If the spleen is where the increased breakdown of platelets takes place, removal of the spleen may be another therapeutic option.
Thrombocytopenia caused by an antibody reaction can also be triggered by an underlying disease. Examples of such underlying diseases are lymph gland cancer, chronic lymphatic leukemia, autoimmune diseases such as systemic lupus erythematosus or the HELLP syndrome that occurs during pregnancy.
The third group of antibody reactions are those triggered by the administration of drugs or blood products. When a certain type of heparin is administered to thin the blood, special antibodies can combine with the platelets and the heparin. This leads to thrombocytopenia and, in severe cases, to thrombosis. After blood transfusions, patients who have already come into contact with exogenous blood, for example after pregnancy or previous blood transfusions, can develop antibodies against their own platelets, which affects them.
Coagulation activation
Excessive coagulation activation occurs, for example, as a complication in shock or sepsis (colloquially blood poisoning), in operations on certain organs or in tumor breakdown. The clotting becomes overly activated and a large number of small blood clots develop. These then block small vessels, which can lead to an undersupply of blood from various organs with subsequent tissue destruction. Because the platelets and the other factors of the coagulation system are used up in a very short time, increased bleeding can occur in the following phase.
A blood test shows a platelet deficiency very early on. Therapy consists of treating the underlying disease. In the early phases of coagulation activation, blood thinning can interrupt the cascade. In later phases, blood should not be thinned, as there is already an increased risk of bleeding, which would only worsen. During these phases, fresh plasma and certain factors in the coagulation system can be replaced via the vein. As a prophylactic measure, blood dilution with heparin should be carried out beforehand in patients who are at risk of coagulation activation.
Find out more about the topic: Bleeding disorder
Mechanical damage to platelets
Platelets can be damaged if they come into contact with non-body surfaces. Mechanical heart valves are an example. They usually consist of a metal and are used as a replacement for the diseased heart valve. Since the mechanical valves do not move like normal heart valves, the platelets can be damaged. The artificial surface can also cause mechanical damage to the platelets.
Another example in which the blood comes into contact with foreign materials is during dialysis. During the procedure, the blood of patients with severe kidney disease is pumped through a special machine and filtered using a membrane. In healthy people this function is taken over by the kidneys. This is where the platelets come into contact with an exogenous surface and can be damaged in this process.
Read more on the topic: dialysis
Distribution disorders
A distribution disorder can be triggered by an enlarged spleen (splenomegaly). The platelets are pooled in the spleen, which means that they collect in the spleen tissue and are therefore not available for the rest of the body's circulation and blood clotting. A blood sample would result in thrombocytopenia because the platelets in the spleen cannot be measured. The platelets are then broken down in the spleen. This breakdown can take on a high rate due to the high number of platelets in the spleen tissue. Another cause of a disturbance in the distribution of platelets is the use of anesthesia which leads to hypothermia.
Laboratory artifact / pseudothrombocytopenia
If a thrombocytopenia is found in the laboratory without any symptoms being noticed beforehand, pseudothrombocytopenia may be present. This can have three causal reasons. Initially, the platelets may have accumulated in the blood tube, which means that they cannot be detected by the measuring devices in the laboratory. This agglomeration can be caused by an incorrect technique when drawing blood.
Another possibility is the presence of certain proteins (EDTA-dependent agglutinins) in the blood tube, which bind to the platelets and thus lead to clumping. In the second case there is an accumulation of white blood cells and platelets. So there is also clumping and the result is again a lower measurable content of platelets in the blood.
The third reason for pseudothrombocytopenia is the presence of so-called giant platelets. The presence of giant platelets can either be congenital or due to various diseases affecting the hematopoietic system. Instead of thrombocytes, the functionless giant platelets are formed, which is why the number of thrombocytes in the laboratory is reduced. Pseudothrombocytopenia can be revealed by using different coated tubes (citrate tubes) or by determining the bleeding time.
alcohol
Heavy alcohol consumption can lead to decreased production of platelets in the bone marrow. This not only disrupts the production of platelets, but also that of the entire bone marrow. As a result, all blood cells may be depleted. The patient then attracts symptoms such as fatigue, small bleeding and susceptibility to infections. The mechanism here is likely to be similar to that of drug-induced thrombocytopenia. However, research is still being carried out into which exact mechanisms are disrupted by alcohol, so that it can damage the bone marrow.
Long-term effects of heavy alcoholism can include white blood cancer or another bone marrow disease. A second mechanism in which excessive alcohol consumption can lead to thrombocytopenia is via the development of liver cirrhosis. Cirrhosis of the liver is caused by long-term damage to the liver from toxic substances such as alcohol. Since liver cirrhosis damages the liver cells, the ability to produce various substances is also reduced. As a result, the liver can only produce an important growth factor for platelets to a lesser extent, which leads to a reduced production of platelets in the bone marrow.
Read more on the topic: Consequences of alcohol